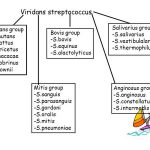
Viridans streptococci have a strong association with bacterial endocarditis (see site) (Box 1). A defectiva and A adjacens were once an important cause of culture-negative endocarditis. However, current laboratory media and techniques enable these “nutritionally variant streptococci” to be identified more readily.