Description of Medical Condition
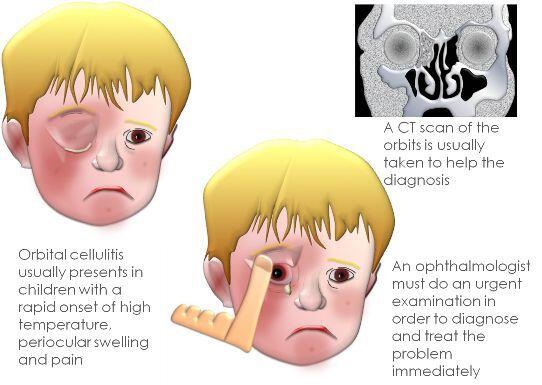
An acute, spreading infection of the dermis and subcutaneous tissue. Several entities are recognized. Cellulitis around the eyes is a potentially dangerous periorbital and orbital infection.
System(s) affected: Skin/Exocrine, Nervous
Genetics: No known genetic pattern
Incidence/Prevalence in USA: Unknown
Predominant age: N/A
Predominant sex: Male = Female
Medical Symptoms and Signs of Disease
- Lid edema
- Rhinorrhea
- Orbital pain, tenderness
- Headache
- Conjunctival hyperemia
- Chemosis
- Ptosis
- Limitation to ocular motion
- Increase intraocular pressure
- Disease in corneal sensation
- Congestion of retinal veins
- Chorioretinal stria
- Gangrene and sloughing of lids
What Causes Disease?
Cellulitis around the eye in adult
- Staphylococcus aureus most common
- Streptococcus pyogenes
- Streptococcus pneumonia
- Mixed infection
Cellulitis around the eye in children less than five years OH. influenzae most common
Risk Factors
- Trauma
- Chronic sinusitis (anaerobic)
- Acute sinusitis (aerobic)
- Retained orbital foreign bodies
- Puncture wound
- Surgical procedure: Exploration of orbital tumor, retinal detachment procedure, strabismus operation
- Acute dacryocystitis
- Dental or intracranial infection
- BacteremiaDiagnosis of Disease
Differential Diagnosis
Retro-orbital cellulitis/abscess
Laboratory
- Aspiration of fluid from the orbit is contraindicated
- Blood culture more likely to be positive in children < 5 years
- Culture of discharge from nasal mucosa, nasopharynx and conjunctiva
Drugs that may alter lab results: Previous antibiotic therapy Disorders that may alter lab results: N/A
Pathological Findings
N/A
Special Tests
Serial serological testing with antistreptolysin, anti-deoxyribonuclease B, and antihyaluronidase tests may be successful in diagnosing cellulitis caused by group A, C, or G hemolytic streptococci
Imaging
- B-scan ultrasound
- Plain orbital and sinus films
- Computerized tomography (CT) is the most accurate and provides the most important information
- Magnetic resonance imaging is the imaging modality of choice in diagnosing suspected cases of cavernous sinus thrombosis
Diagnostic Procedures
- Skin biopsy
- Lumbar puncture should be considered for all children with H. influenzae type B cellulitis
Treatment (Medical Therapy)
Appropriate Health Care
Outpatient for mild cases, inpatient for severe infections
General Measures
N/A
Surgical Measures
- Surgical debridement and/or drainage is needed if abscess develops or if clinical situation deteriorates despite adequate therapy in 24-48 hours or if visual acuity decreases
- In orbital mucormycosis, surgical debridement of devitalized tissue is extremely important
Activity
- Ambulatory in mild infection
- Bedrest in severe infection
Diet
Regular diet
Patient Education
- Good skin hygiene
- Avoid skin traumas
- Report early skin changes to health professional
Medications (Drugs, Medicines)
Drug(s) of Choice
- In adults, nafcillin or oxacillin 1.5 g every 4 hours
- In children, ampidllin 200 mg/kg/day in divided doses intravenously plus nafcillin or oxacillin (100 mg/kg/day)
- Sinus decongestion — nasal sprays, oral decongestants. oral antihistamines
Contraindications:
- Allergies to the antibiotic
- Previous history of allergy to the drug
Precautions: Renal failure, other organ failure Significant possible interactions: Refer to manufacturer’s literature
Alternative Drugs
- In adults, cefotaxime or clindamycin or chloramphenicol orvancomycin
- In children, influenzae resistant to ampicillin third generation cephalosporin, cefotaxime or chloramphenicol
- In immunocompromised — piperacillin and gentamicin
- Fluoroquinolones (adults)
- Linezolid (Zyvox)
Patient Monitoring
Repeat imaging in patients with orbital cellulitis
Prevention / Avoidance
- Avoid trauma
- Avoid swimming in fresh water or salt water in the presence of skin abrasion
- In influenzae cellulitis — rifampin prophylaxis for the entire family of an index case. Rifampin prophylaxis in day-care classroom in which one or two children exposed. Dosage — 20 mg/kg/24 h (maximum of 600 mg a day) for 4 days.
Possible Complications
- Osteomyelitis
- Strabismus
- Afferent pupillary defect
- Chronic draining sinus
- Scarred upper eyelid
- Profound visual loss
- Blindness
- Ophthalmoplegia
- Cavernous sinus thrombosis
- Meningitis
- Intracranial abscess
- Acute infarction of retina and choroid
Expected Course / Prognosis
With adequate antibiotic treatment, outlook is good
Miscellaneous
Associated Conditions
Sinusitis ethmoiditis in children in 84% of patients
Age-Related Factors
Pediatric: Newborn may acquire orbital cellulitis secondary to intrauterine infection Geriatric: N/A
Pregnancy
N/A
International Classification of Diseases
376.01 Orbital cellulitis
See Also
Cellulitis Erysipelas Animal bites Thrombophlebitis, superficial