Essentials of Diagnosis
- Patients present with watery diarrhea, which is usually self-limited in immunocompetent patients but may be prolonged in the immunocompromised patient.
- A history of travel to areas such as Nepal, Haiti, and Peru, a history of berry consumption, or community outbreak of diarrhea may increase suspicion of diagnosis.
- Acid-fast stain of stool specimens reveals abundant oocysts.
General Considerations
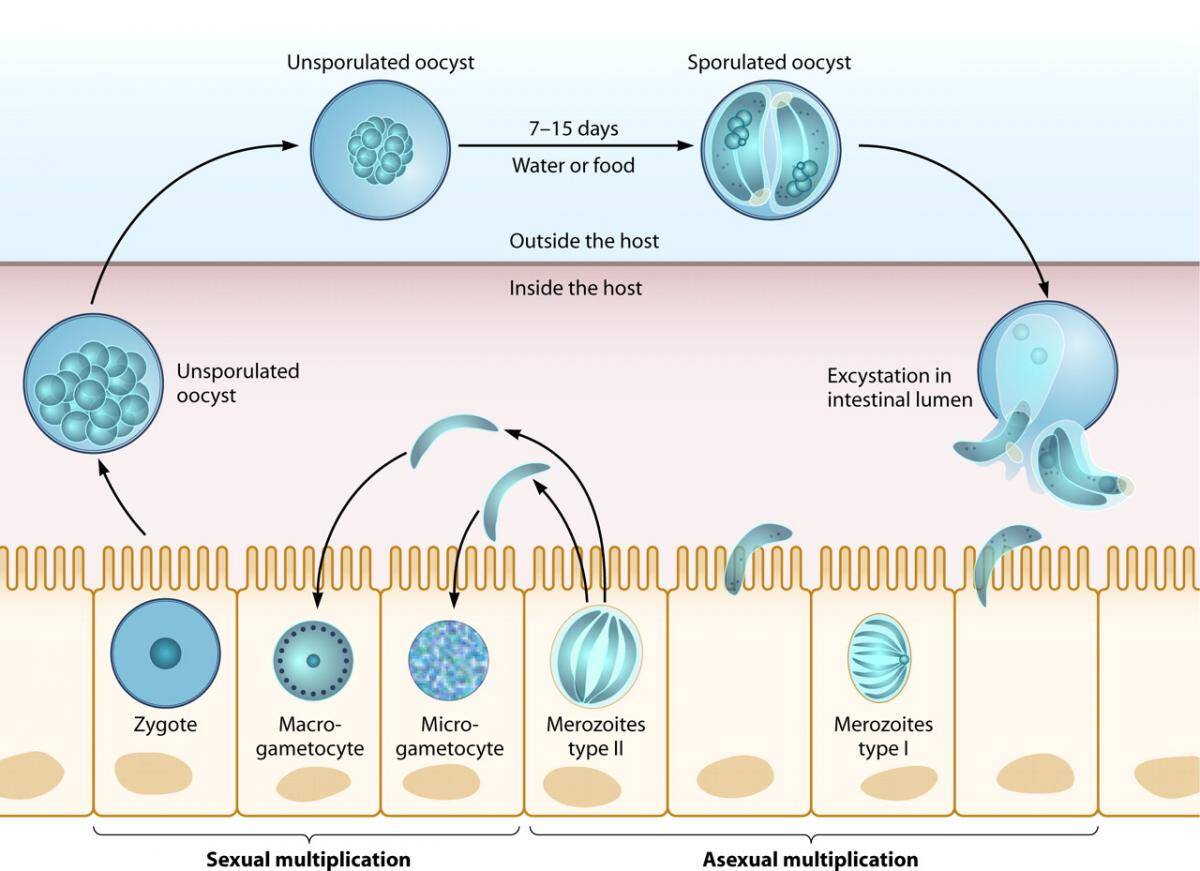
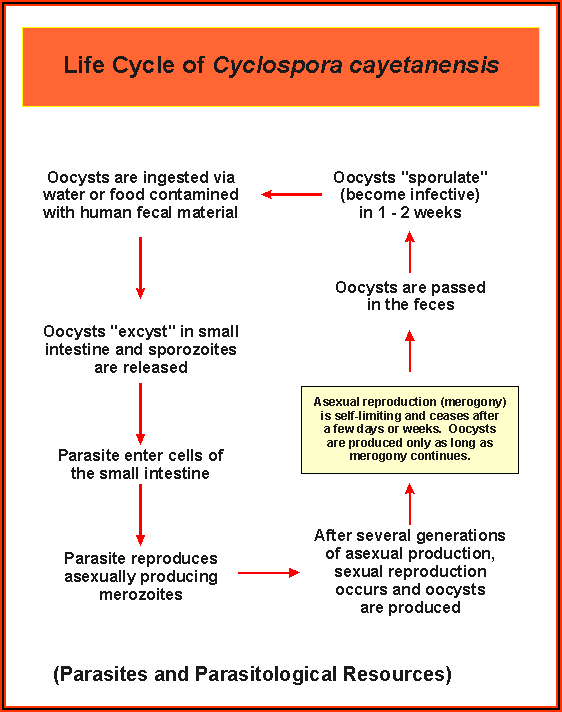
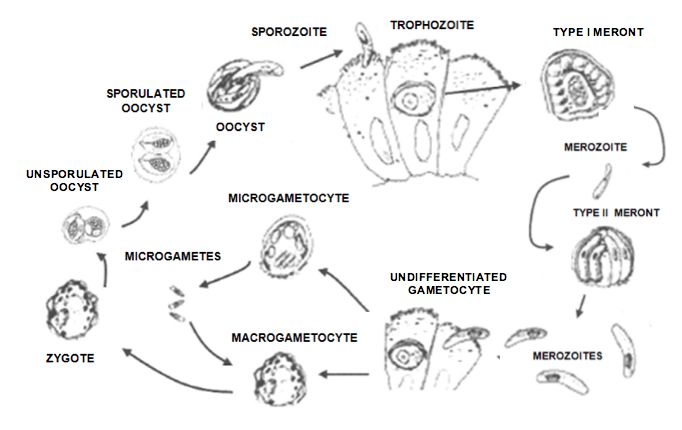
Cyclospora is a coccidian that had been described as a “large cryptosporidium” or “cyanobacterium-like body” before being confirmed as a member of the phylum Apicomplexa in 1993. The life cycle in humans has not been fully detailed. The organism has been shown to infect jejunal enterocytes. Similar to Isospora, the oocysts are excreted unsporulated, requiring 7-13 days of optimal conditions outside of the host to mature. Each spherical oocyst has a diameter of 8-10 um and contains two sporocysts, each of which contains two sporozoites. The oocyst is twice the size of C parvum.
Cyclospora catayensis infection in humans has been reported worldwide and was first described in Papua New Guinea in 1979. It is endemic in Haiti, Peru, and Nepal, where rainy-season outbreaks of C catayensis infection occur. Outside these areas, infection is usually travel related when not associated with an outbreak. Protective immunity is suggested because infection is more common in children and in non-natives. Infection has been reported in HIV-infected patients, but cyclosporiasis is primarily found in immunocompetent patients. In the United States, Cyclospora oocysts were identified in only 3 of 1042 submitted stools. The low prevalence in patients with AIDS in the United States is attributed to possible misdiagnoses as C parvum, nonuniform use of the acid-fast stain, trimethoprim-sulfamethoxazole (TMP-SMX) prophylaxis in these patients, and the coincident low prevalence in immunocompetent patients in the United States.
Transmission of Cyclospora has been linked to contaminated water and food sources. The organism is believed to be host specific to humans. In 1990, a Chicago outbreak was related to stagnant water in a storage tank, and in 1994, in Nepal, a British military unit experienced an outbreak related to water from a chlorinated and filtered tank. More recently, cyclosporiasis related to berry consumption has been in the news. In 1995, unwashed strawberries were related to outbreaks in New York and Florida. In 1996, 1465 cyclosporiasis cases in two Canadian provinces and 20 states in the United States were traced to consumption of Guatemalan raspberries. Lettuce and uncooked meat have been reported culprits as well.
The pathogenesis of cyclosporiasis is not well understood. The parasite is found in the upper small bowel and is associated with villous atrophy, crypt hyperplasia, and inflammatory changes similar to those seen in tropical sprue.
Clinical Findings
After an incubation of 2-11 days, immunocompetent patients experience a self-limited, but prolonged, relapsing watery diarrhea lasting an average of 19-43 days, although organism shedding may last = 70 days (Box 4). In patients with AIDS, symptoms have been reported for = 4 months. A median of six stools/day is reported. Fatigue, fever, indigestion, abdominal cramps, nausea, and vomiting may occur, as well as weight loss. A prodrome of both myalgia and arthralgia has been reported. Diarrhea may not be the primary complaint, and alternation with constipation is not infrequent. Asymptomatic infection has been reported in a study of immunocompetent Peruvians with documented infection in whom only 11-28% had diarrhea. No specific laboratory findings assist in diagnosis although abnormal D-xylose absorption has been reported.
Differential Diagnosis
A similar presentation may be found in cryptosporidiosis, isosporiasis, microsporidiosis, and sarcocystosis.
Complications
Biliary disease has been reported.
Diagnosis
Diagnosis is made by identification of the Cyclospora oocyst in fresh or iodine-preserved stool, duodenal aspirates, or small-bowel biopsies. With acid-fast or safranin O staining, oocysts can be seen as 10 um spheres with clusters of refractile globules. The oocysts autofluoresce blue under UV light with a 365-nm excitation filter (Table 2).
Treatment
TMP-SMX is the first-line treatment for cyclosporiasis, with symptom resolution noted 2-3 days into therapy (Box 5). Immunosuppressed patients may require long-term suppressive therapy owing to an increased relapse rate. In addition to TMP-SMX, metronidazole, tinidazole, and ciprofloxacin hydrochloride have also been reported to stop oocyst excretion.
Prognosis
Infection is generally self-limited in immunocompetent hosts, but prolonged diarrhea with possible symptoms of malabsorption may occur in immunocompromised patients.
Prevention & Control
Reliable means of prevention of Cyclospora spp. infection are not yet known (Box 6). Efforts to decrease berry contamination have been directed toward using potable water in all aspects of berry preparation, including water used for insecticide spray and for hand washing by workers. Gamma radiation used on berries is also being studied.