General Considerations
Epidemiology
The epidemiology of rubella, commonly referred to as German measles or 3-day measles, has changed dramatically in the past 30 years, owing exclusively to the widespread use of the rubella live attenuated virus vaccine. Before the use of this vaccination (1969), the virus had an epidemic cycle of 6-9 years. It is primarily a winter and early spring infection. The incidence of rubella infection in developed countries has declined by 99%, compared with pre-vaccine era data. In the vaccine era, current data suggest that 10% of young adults are still susceptible. The majority of these young adults lack vaccination.
A major concern of rubella is infection of nonimmune pregnant women. Polysystemic fetopathy is the hallmark of congenital rubella syndrome. Infection before 20 weeks of gestation confers a significant risk of congenital malformation with the highest risk before 12 weeks of gestation.
Microbiology
Rubella is a 70-nm single-stranded RNA virus of the Togaviridae family. It is the only virus in the genus Rubivirus. It has three polypeptide constituents (E1, E2, and C). E1 and E2 are glycosylated membrane peptides. The nucleocapsid is composed of polypeptide C and genomic RNA. The viral envelope is a lipoprotein complex. The virus is sensitive to heat, light, and pH extremes.
Pathogenesis
Humans are the only natural reservoir of the virus. Spread is chiefly via respiratory secretions and direct contact. The virus is communicable for 3-5 days before the rash and 7 days after the rash has appeared. The virus has a latent phase of 2-3 weeks before clinical disease appears.
POSTNATALLY ACQUIRED RUBELLA
Essentials of Diagnosis
- Exanthematous viral illness.
- A prodrome of cough, fever, myalgia, cervical lymphadenopathy, and pharyngitis is common in adults.
- Prodrome is rare in children.
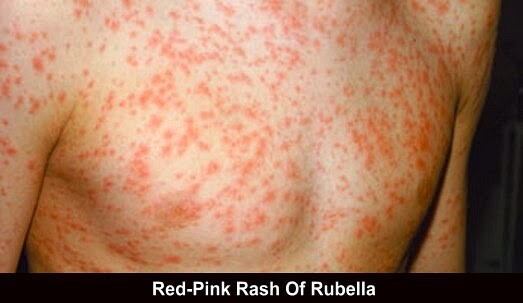
- Exanthem is a fine maculopapular rash spreading from the face to the extremities within 24 h and lasting 3 days.
- Nonimmune pregnant women are at high risk for having a fetus with congenital rubella syndrome.
Clinical Findings
Signs and Symptoms
Postnatal infection is usually a mild illness accompanied by an exanthem rash (Box 1). Adults commonly have prodromal symptoms including pharyngitis, fever, headache, cough, lymphadenopathy, myalgia, and nausea for 1-5 days. Children rarely have a prodrome.
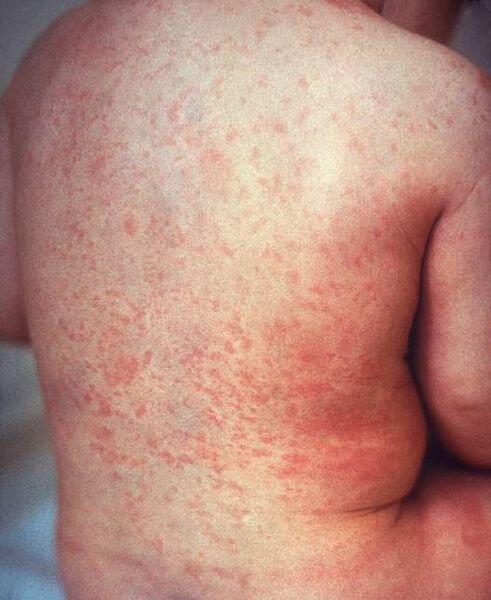
The exanthem is similar in adults and children. The erythematous, fine maculopapular rash first erupts on the face, then spreads to the distal extremities within 24 h and lasts 2-3 days. In children, the exanthem phase has little to no fever. Lymphadenopathy is common, as is mild, transient leukopenia. The exanthem phase in adults commonly involves arthritis, headache, and eye pain. Generalized pruritus may last 2 weeks.
Laboratory Findings
Culture may be obtained from nasopharyngeal secretions, blood, urine, cerebrospinal fluid, synovial fluid, and breast milk. The preferred medium is African green monkey kidney cells. No reliable clinical viral antigen test exists. Serology is performed via hemagglutination inhibition, latex agglutination, fluorescence immunoassay, passive hemagglutination, single radial hemolysis, and enzyme immunoassay. Serology should be performed on a suspected case. Absence of immunoglobulin G (IgG) indicates nonimmunity. Repeat serology at 4 and then 6 weeks. Seroconversion is indicative of infection.
Differential Diagnosis
The differential diagnosis includes measles, fifth disease, roseola, scarletina, and infectious mononucleosis.
Complications
Complications for children include encephalitis and thrombocytopenia. Adults can have myocarditis, orchitis, neuritis, erythema multiforme, and congenital rubella syndrome.
Diagnosis
Postnatally acquired rubella is diagnosed based on history and physical findings (see Box 1). All suspected cases that are nonimmune should have cultures and serology performed to confirm the diagnosis. If serology shows no rubella-specific IgG (eg, nonimmune), convalescent titers should be drawn at 4 and then 6 weeks postexposure. Seroconversion is indicative of active infection. If active infection is identified in a nonimmune pregnant woman before 20 weeks’ gestation, pregnancy termination should be discussed. The patient’s religious, cultural, and personal values must be considered in this situation. Infection after 20 weeks gestation has a decreased risk of teratogenic effects on the fetus.
Treatment
Postnatally acquired rubella requires no specific treatment. Therapy should be symptomatic (Box 2). Use of immunoglobulin as postexposure prophylaxis in nonimmune patients is controversial. Routine administration of immunoglobulin for postexposure prophylaxis of rubella is not recommended. Symptoms in the mother may be reduced, but fetopathy may still occur. Immunoglobulin may be considered in cases where pregnancy termination was indicated but not possible.
CONGENITAL RUBELLA SYNDROME
Essentials of Diagnosis
- Polysystemic fetopathy.
- Infection before 20 weeks’ gestation confers greatest risk to fetus.
- Common defects include cataracts, deafness, microcephaly, heart defects, hepatosplenomegaly.
- Late complications include mental retardation, developmental and behavioral disorders, endocrinopathies.
- Infant will shed virus up to 1 year.
Clinical Findings
Nonimmune pregnant women infected with rubella are at risk for having a fetus with congenital rubella syndrome (CRS). The risk and severity of the defects are higher earlier in the pregnancy. Roughly 85% of fetuses infected in the first trimester will have some anomalies.
Hallmarks of CRS include sensorineural deafness, intrauterine growth retardation, cataracts, retinopathy, and cardiac defects (Box 3). Some infections will result in spontaneous abortion. Uncommon findings also include dermal erythropoiesis, meningoencephalitis, glaucoma, microphthalmia, myocarditis, pneumonitis, hepatitis, thrombocytopenic purpura, and craniofacial deformities. Many of these infants will grow to have mental retardation, developmental delay, and behavioral disorders. Some will also have late-onset endocrinopathies such as insulin-dependent diabetes mellitus. The virus can be isolated as outlined above.
Diagnosis
CRS is diagnosed based on history and physical findings (see Box 3). Some neonates, especially those affected later in pregnancy, may appear normal or have very mild findings at birth. Suspected CRS neonates should have a rubella-specific IgM drawn. Cultures should be obtained from nasal secretions, blood, urine, and cerebrospinal fluid.
Treatment
No medical therapy is available for CRS (but see Box 2). Cardiac defects warrant early intervention by a pediatric cardiologist. Early audiologic evaluation should be performed. A physician experienced with patients who have developmental disabilities should be involved. Early intervention for developmental delays and mental retardation is important. The primary care provider should be aware of potential endocrinopathies. Children with CRS often have very difficult behavioral disorders. Parents will benefit from behavioral management counseling.
Prevention & Control of Rubella
Rubella is communicable 3-5 days before the rash and = 7 days after it appears in postnatally acquired cases. Hospitalized patients should be in droplet isolation. Pregnant hospital staff should avoid contact if their immunity status is in question. Infected children should be excluded from school and daycare during this period. CRS infants may shed the virus for = 1 year. Parents should be aware of this factor and restrict the infant’s exposure to pregnant women.
Universal vaccination has been key in reducing the occurrence of CRS. Prenatal screening of pregnant women’s immunity status has also been important. Rubella immunization is usually given in combination with the MMR (measles, mumps, rubella) vaccine. The first vaccine should be given at 12-15 months of age. The second should be given at 4-6 years of age. If the second dose is missed, it should be given before 12 years of age. Various contraindications and precautions exist for the vaccine (Box 4).
BOX 1. Postnatally Acquired Rubella
Children
Adults
Prodromal Symptoms
- Prodromal symptoms are rare
- Cough, coryza, lymphadenopathy, and diarrhea
- Prodromal symptoms are common
- Eye pain, sore throat, headache, fever, cough, lymphadenopathy, myalgia, and nausea
Rash
- Initial presentation is exanthem rash
- Rash is erythematous, maculopapular; found first on the face then spreading peripherally within 24 h
- Rash occurs 1-5 days after prodromal symptoms appear
- Rash is similar to children’s rash
- Usually lasts 2 to 3 days
Exanthem Phase
- Fever is mild to none
- Arthritis and arthralgia are common
Clinical Signs
- Lymphadenopathy is common, typically posterior auricular
- Mild, transient leukopenia
- Lymphadenopathy is common, typically posterior auricular and suboccipital and suboccipital
- Persistent headache, eye pain, and pruritus may last for = 2 weeks.
Rare Complications
- Encephalitis
- Thrombocytopenia
- Myocarditis
- Erythema multiforme
- Congenital rubella syndrome
BOX 2. Treatment of Rubella Infection
Congenitally
Infected Neonates
Children
(Postnatal Infection)
Adults
Nonimmune Pregnant Women
- Specific IgM should be drawn
- Cultures taken from nasal secretion, blood, urine, & cerebrospinal fluid
- Auditory assessment
- Early intervention for developmental and behavioral disorders
- No medical therapy available
- Supportive care
- Manage fever with acetaminophen (10-15 mg/kg every 4 h orally or rectally) or ibuprofen (6 to 8 mg/kg every 6 to 8 h orally)
- Supportive care
- Analgesia with NSAIDs
- Antihistamines for pruritus
- Draw blood for rubella-specific IgG immediately to identify immunity status
- If no identifiable IgG, repeat serology should be drawn in 4 and 6 weeks; seroconversion indicates acute infection
- Use of immunoglobulin for postexposure prophylaxis is controversial; 0.55 cc/kg may modify infection; this is not recommended
- If confirmed infection before 20 weeks gestation, pregnancy termination should be considered
BOX 3. Congenital Rubella Syndrome
More Common Findings at Birth
- Intrauterine growth retardation
- Cataracts
- Retinopathy
- Sensorineural deafness
- Microcephaly
- Long bone radiolucencies
- Patent ductus arteriosus
- Pulmonary artery stenosis
- Hepatosplenomegaly
- Dermal erythropoiesis (producing the “Blueberry Muffin” appearance)
Less Common Findings at Birth
- Active meningoencephalitis
- Congenital glaucoma
- Microphthalmiax
- Myocarditisx
- Interstitial pneumonitisx
- Hepatitisx
- Thrombocytopenia purpurax
- Craniofacial abnormalities
Late Complications
- Mental retardation
- Developmental delay
- Behavioral disorders
- Endocrinopathies
BOX 4. Control of Rubella
Vaccine
- Live attenuated virus rubella vaccine (RA 27/3 strain) is administered 0.5 cc SQ. Commonly given in combination with MMR (measles, mumps, rubella) vaccine
- First dose is recommended from 12 to 15 months of age
- Second dose is recommended at school entry (age 4 to 6 years)
- If no preschool dose is given, the second dose should be administered prior to age 12
- Susceptible persons should be screened for immunization status; these include prepubertal girls & boys, college students, military personnel, child care workers, health care workers, postpartum women
MMR Vaccine Contraindications
- Pregnancy
- Febrile illness
- Planned pregnancy within 3 months
- Severe immunocompromised state
- Blood product or immune globulin within 3 to 6 months (dose dependent)
- Anaphylaxis to neomycin
MMR Vaccine Should Be Used with Caution in These Situations
- Seizure disorder
- Thrombocytopenia
- Egg allergy
Isolation Precautions
- Postnatally acquired rubella requires respiratory isolation for 5 days before the rash through 1 week after appearance of the rash; this includes exlusion from school or daycare
- Congenitally infected infants are considered contagious until 1 year of age unless nasal and urine cultures are negative at 3 months; parents must be made aware of the potential risk to nonimmunized pregnant mothers

