Essentials of Diagnosis
- Increased risks in promiscuous homosexual men, travelers to underdeveloped areas, and institutionalized individuals.
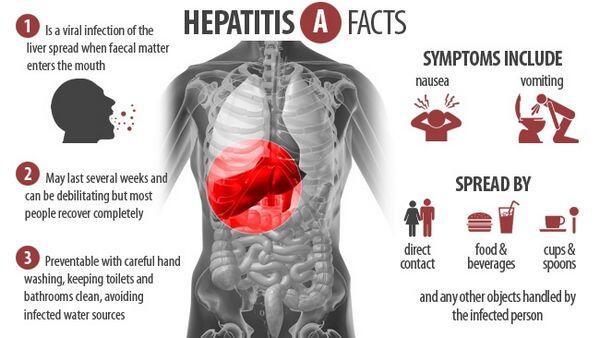
- Malaise, anorexia, fever, dark urine, pale stools, jaundice, right upper quadrant pain, and tender hepatomegaly.
- Increased liver enzymes (ALT, AST), bilirubin, prothrombin time, and globulin.
- Serum positive for hepatitis A immunoglobulin M (IgM) antibody.
- May have history of recent (ie, 3-6 weeks previously) ingestion of undercooked shellfish or sewage-contaminated water.
General Considerations
Epidemiology
Hepatitis A virus is the cause of what was formerly termed infectious hepatitis or short-incubation hepatitis. It was first detected in the early 1970s in stools of patients incubating the disease. Humans appear to be the major natural hosts of hepatitis A virus. Several other primates (including chimpanzees and marmosets) are susceptible to experimental infection, and natural infections of these animals may occur.
The major mode of spread of hepatitis A is fecal-oral. Inoculation of infectious material intramuscularly can produce disease; transmission through blood transfusion rarely, if ever, occurs. Most cases of hepatitis A occur sporadically rather than being linked to a single contaminated source. The disease is common under conditions of crowding, and it occurs at high frequency in mental hospitals, schools for the developmentally disabled, and daycare centers. Because a chronic carrier state has not been observed with hepatitis A, perpetuation of the virus in nature presumably depends on sporadic subclinical infections and person-to-person transmission. Outbreaks of hepatitis A have been linked to the ingestion of undercooked shellfish from waters contaminated with human feces. Common-source outbreaks related to other foods, including vegetables, have also been reported.
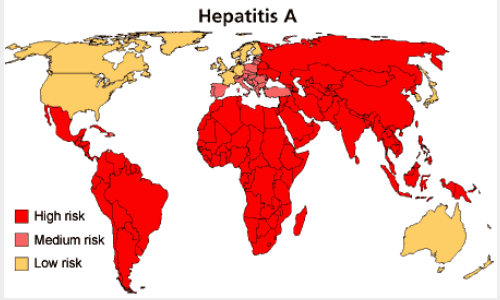
The disease is widespread, but seroepidemiologic studies have shown marked variation in infection rates among different population groups. For example, rates are higher among those of lower socioeconomic status and among male homosexuals. Less than one-half of the general population of the United States now has serologic evidence of prior hepatitis A virus infection. Rates have been decreasing since 1970, apparently because of better sanitation and less crowding. In contrast, in many underdeveloped countries, > 90% of the adult population shows evidence of previous hepatitis A infection; in most cases, however, the evidence is of asymptomatic infection during childhood. The risk of overt disease is much higher in nonimmune infected adults than in children; travelers from developed countries who enter endemic areas are particularly susceptible.
Microbiology
Hepatitis A virus is an unenveloped, single-stranded small RNA (picorna)virus with cubic symmetry and a diameter of 27 nm. It is not inactivated by ether and is stable at -20 °C and low pH. These properties are similar to those of enteroviruses (see site), but hepatitis A virus is distinct and now classified in a separate genus, Hepatovirus. The virus has been successfully cultivated in cell cultures but grows poorly.
Pathogenesis
The virus is believed to replicate initially in the enteric mucosa. It can be demonstrated in feces by electron microscopy for 10-14 days before onset of disease. In most patients with symptoms of the disease, complete virus is no longer found in fecal specimens; however, viral antigen has been demonstrated in feces for = 14 days thereafter. Multiplication in the intestines is followed by a period of viremia with spread to the liver. The response to replication in the liver consists of lymphoid cell infiltration, necrosis of liver parenchymal cells, and proliferation of Kupffer cells. The extent of necrosis often coincides with the severity of disease. A variable degree of biliary stasis may be present. Detectable levels of IgG antibody to hepatitis A virus persist indefinitely in serum, and patients with anti-hepatitis A virus antibodies are immune to reinfection.
Clinical Findings
Signs and Symptoms
In hepatitis A virus infection, an incubation period of 10-50 days (mean, 25 days) is usually followed by the onset of fever, poor appetite, nausea, pain in the right upper abdominal quadrant, and, within several days, jaundice. The patient may notice dark urine and clay-colored stools 1-5 days before the onset of clinical jaundice. The liver is enlarged and tender. Many persons who have serologic evidence of acute hepatitis A infection are asymptomatic or only mildly ill, without jaundice (anicteric hepatitis A). The infection-to-disease ratio is dependent on age; it may be as high as 20:1 in children and approximately 4:1 in adults. Most (99%) of cases of hepatitis A are self-limiting.
Laboratory Findings
Serum aminotransferase levels are elevated as a result of hepatic inflammation and damage. The serum bilirubin levels and prothrombin time are also elevated, the latter being a sensitive marker of hepatocyte damage. The total leukocyte count is low because of neutropenia. Alkaline phosphatase is elevated especially in patients with a cholestatic picture, but it tends to subsequently decrease even when the bilirubin is still rising.
Imaging
Radiographic and radionucleotide studies may show hepatomegaly. Gall bladder and common bile duct examinations are usually normal.
Differential Diagnosis
All of the causes of acute hepatitis mentioned in the introduction to this SITEmust be considered, but epidemiologic, age, and risk factors may help to predict a probable cause. See also Table 3.
Complication
In 0.1% of cases, fulminant fatal hepatitis associated with extensive liver necrosis may occur.
Diagnosis
The best method for documentation of acute hepatitis A virus infection is the demonstration of high titers of virus-specific IgM antibody in serum drawn during the acute phase of illness. Because IgG antibody persists indefinitely, its demonstration in a single serum sample is not indicative of recent infection; a rise in titer between acute and convalescent sera must be documented. Immune electron microscopic identification of the viral antigen in fecal specimens and isolation of the virus in cell cultures remain research tools. Past infection is best demonstrated by anti-HAV IgG but absent IgM.
Treatment
There is no specific treatment for patients with acute episodes of hepatitis A infection (Box 2). Supportive measures include adequate nutrition and rest.
Prognosis
The prognosis is excellent for > 99% of patients with hepatitis A infection. Only 0.1% of patients develop fatal acute hepatic necrosis.
Prevention & Control
Passive Immunization
Passive (ie, antibody) prophylaxis for hepatitis A has been available for many years. Immune serum globulin (ISG), manufactured from pools of plasma from large segments of the general population, is 80-90% protective if given before or during the incubation period of the disease. In some cases, infection occurs, but disease is ameliorated; that is, the patient develops anicteric, usually asymptomatic, hepatitis A.
At present, ISG should be administered to household contacts of hepatitis A patients and those known to have eaten uncooked foods prepared or handled by an infected individual. Once clinical symptoms have appeared, the host is already producing antibody, and administration of ISG is not indicated. Persons from areas of low endemicity who travel to areas with high infection rates may receive ISG before departure and at 3- to 4-month intervals as long as potential heavy exposure continues, but active immunization is preferable (see below).
Active Immunization
For hepatitis A, live attenuated vaccines have been evaluated but have demonstrated poor immunogenicity and have not been effective when given orally. Formalin-killed vaccines induce antibody titers similar to those of wild-virus infection and are almost 100% protective. Use of this vaccine is preferable to passive prophylaxis for those with prolonged or repeated exposure to hepatitis A.

