Description of Medical Condition
An inflammation of the uterine cervix.
- Infectious cervicitis may be caused by Chlamydia trachomatis, Neisseria gonorrhoeae, Mycoplasma genitalium, ureaplasmas, Herpes simplex or Trichomonas vaginalis.
- Chronic cervicitis is characterized by inflammation of the cervix without an identified pathogen
System(s) affected: Reproductive Genetics: N/A Incidence/Prevalence in USA:
- Gonorrhea: 166/100,000; 2% of sexually active women < age 30
- Chlamydia: 290/100,000; 5-35% of women
- Trichomonas: 1200/100,000; 5-25% of women
Predominant age: Infectious cervicitis is most common in adolescents, but can be seen in women of any age
Predominant sex: Female only
Medical Symptoms and Signs of Disease
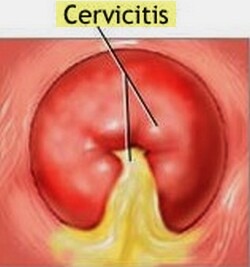
- Mucopurulent (yellow) discharge from the cervix
- Cervical erosion or erythema
- Easily induced endocervical mucosal bleeding
- Tenderness of cervix
- Postcoital bleeding
- Frequently asymptomatic
What Causes Disease?
- Chlamydia trachomatis
- Neisseria gonorrhoeae
- Herpes simplex virus
- Trichomonas vaginalis
- Mycoplasmas
- Ureaplasmas
- Cytomegalovirus
- Unknown and other pathogens
Risk Factors
- Multiple sexual partners
- History of sexually transmitted disease
- Postpartum period
Diagnosis of Disease
Differential Diagnosis
- Vaginal infections with Candida albicans or Trichomonas vaginalis extending onto the cervix
- Carcinoma of the cervix
Laboratory
- Endocervical gram stain, more than 10 WBC’s per high power field (hpf) suggests cervicitis
- Cervical cultures for C. trachomatis, N. gonorrhoeae
- Polymerase chain reaction (PCR) and ligase chain reaction (LCR) more sensitive than cultures for chlamydia. LCR can be used with urine.
- Enzyme immunoassays (ElAs) of endocervical swabs for chlamydia and gonorrhea
- Nucleic acid amplification tests (NAATs) are more sensitive and can also be used on urine specimens
- Wet mount for Trichomonas vaginalis
- If ulcerations present, culture for herpes simplex virus
- Venereal Disease Research Laboratory (VDRL) or rapid plasma reagin (RPR) to rule out concurrent syphilis
Drugs that may alter lab results: Recent antibiotic treatment Disorders that may alter lab results: N/A
Pathological Findings
Inflammatory changes on Pap smear
Diagnostic Procedures
Colposcopy is indicated in chronic inflammation, with biopsy of suspicious areas
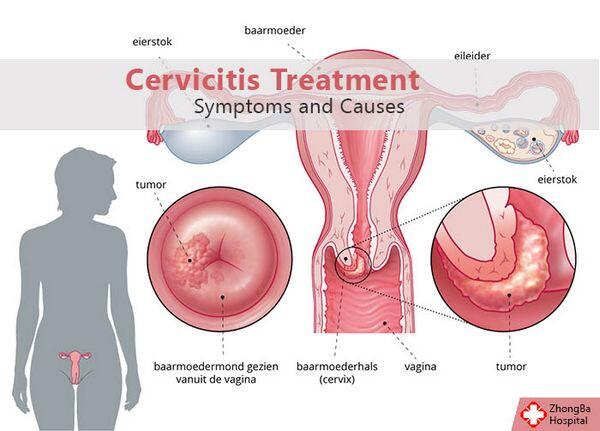
Treatment (Medical Therapy)
Appropriate Health Care
Outpatient treatment
General Measures
Chronic cervicitis with negative cultures and biopsies may be treated with cryosurgery
Activity
Full activity
Diet
No special diet
Patient Education
- Advise patient to use condoms consistently
- If infectious etiology, advise patient to inform her partners about their need for treatment
Medications (Drugs, Medicines)
Drug(s) of Choice
- If infectious cervicitis suspected, treat without awaiting culture results. Ceftriaxone (Rocephin) 125 mg IM single dose; followed by either doxycycline (Vibramycin) 100 mg po bid for 7 days or azithromycin (Zithromax) 1 g single dose.
- For trichomonas, metronidazole (Flagyl) 2 g single dose
- For herpes, acyclovir (Zovirax) 200 mg po 5 times daily (or 400 mg tid) for 7 days
- Chronic cervicitis associated with postmenopausal vaginal atrophic changes may respond to topical estrogen creams
Contraindications:
- Doxycycline should not be used in pregnant or nursing mothers
Precautions: Doxycycline should not be taken with milk, antacids, or iron containing preparations Significant possible interactions: Doxycycline — warfarin (Coumadin) and oral contraceptives may have their effectiveness reduced
Alternative Drugs
- Any of the following can be substituted for ceftriaxone (quinolones should not be used for gonorrhea in patients who have traveled to Hawaii, California, or Southeast Asia because of high levels of resistance)
- Ofloxacin (Floxin) 400 mg po single dose
- Ciprofloxacin (Cipro) 500 mg po single dose
- Levofloxacin (Levaquin) 250 mg single dose
- Erythromycin base or stearate 500 mg po qid, or erythromycin ethylsuccinate 800 mg po qid can be substituted for doxycycline
Patient Monitoring
- Repeat cultures after treatment for chlamydia or gonorrhea are indicated in pregnant or high risk patients
- Annual Pap smears in sexually active patients screen for chronic cervicitis
Prevention / Avoidance
Patients with more than one sexual partner should be advised to use condoms at every encounter
Possible Complications
- Cervicitis with C. trachomatis or V. gonorrhoeae is associated with an 8-10% risk of subsequent pelvic inflammatory disease
- Moderate to severe inflammation is associated with condyloma acuminatum and cervical carcinoma
Expected Course / Prognosis
- Infectious cervicitis usually responds to systemic antibiotics
- Chronic cervicitis may be resistant to treatment, and should be monitored closely for cervical dysplasia
Miscellaneous
Associated Conditions
Patients with infectious cervicitis should be screened for other sexually transmitted diseases, syphilis, trichomonas, and possibly human immunodeficiency virus (HIV)
Age-Related Factors
Pediatric: Infectious cervicitis in children should lead to investigation for possible sexual abuse Geriatric:
- Chronic cervicitis in postmenopausal women may be related to lack of estrogen
- The possibility of infectious cervicitis should not be overlooked, as many geriatric patients remain sexually active
Others: Adolescents remain a high-risk group for sexually transmitted diseases
Pregnancy
Screen all pregnant women for infectious cervicitis because of the risk of transmission to the fetus
Synonyms
Mucopurulent cervicitis
International Classification of Diseases
616.0 Cervicitis and endocervicitis 098.15 Acute gonococcal cervicitis 079.88 Chlamydia infection 099.53 Other venereal diseases due to Chlamydia trachomatis, lower genitourinary sites
See Also
- Chlamydial sexually transmitted diseases
- Gonococcal infections
- Trichomoniasis
- Cervicitis, ectropion & true erosion
- Cervical dysplasia
Other Notes
The presence of trichomonas does not rule out other concurrent infection






