Description of Medical Condition
A common disease transmitted by inhaling airborne bacilli from a person with active tuberculosis (TB). The bacilli multiply in the alveolus and are carried by macrophages, lymphatics and blood to distant sites (eg. lung pleura, brain, kidney and bone). Tissue hypersensitivity usually halts infection within 10 weeks.
- Latent tuberculosis infection (LTBI) is asymptomatic, noninfectious and usually detected by a positive skin test
- TB: active disease — occurs in 10% of infected individuals without preventive therapy. Chance of disease increases with immunosuppression and is highest for all individuals within 2 years after infection — 85% of cases are pulmonary which is infectious.
- Primary TB: disease resulting from the initial pulmonary infection which the immune system is unable to control
- Recrudescent TB: active disease occurring after a period of latent asymptomatic infection
- Miliary TB: disseminated disease
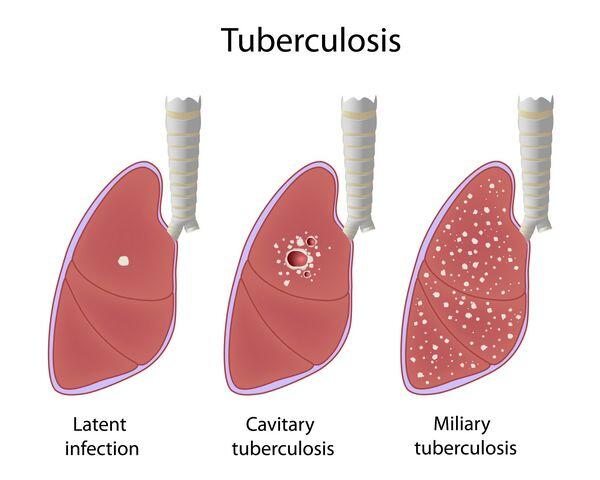
System(s) affected: Pulmonary, Hemic/Lym-phatic/lmmunologic, Renal/Urologic, Gastrointestinal, Nervous, Endocrine/Metabolic, Musculoskeletal
Genetics: N/A
Incidence/Prevalence in USA: Decreasing overall incidence of TB: 5.1/100,0000, but greater among high risk
Predominant age:
- Primary infection — any age, especially pediatric
- Recrudescent disease — adults and elderly
Predominant sex: Male > Female
Medical Symptoms and Signs of Disease
- Cough
- Hemoptysis
- Fever and night sweats
- Weight loss
- Malaise
- Adenopathy
- Pleuritic chest pain
- Hepatosplenomegaly
- Renal, bone or CNS disease are late findings
What Causes Disease?
Mycobacterium tuberculosis, Mycobacterium bovis, and Mycobacterium africanum
Risk Factors
- For infection: Urban, homeless, minority, migrant workers; institutional (eg, prison, nursing home); close contact with infected individual; immigrant within 5 years (Asia, Africa, Latin America); healthcare workers
- For disease: HIV; recent infection; IV drug abuse; lymphoma; diabetes mellitus; chronic renal failure malnutrition; steroids, immunosuppressive drugs; silicosis; gastrectomy; cancer of head, neck or lung, tumor necrosis factor antagonists
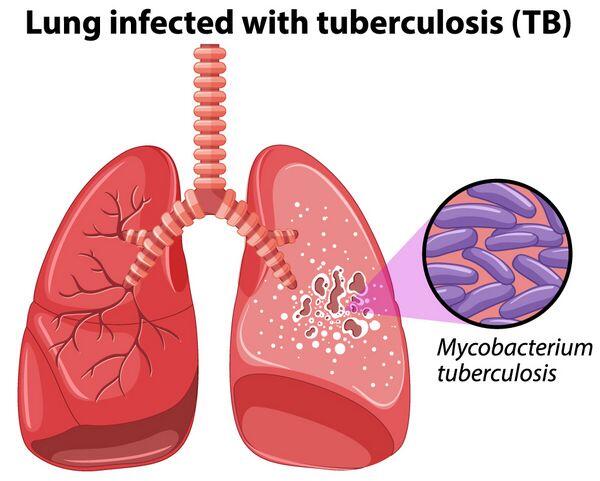
Diagnosis of Disease
Differential Diagnosis
- Other pneumonias
- Lymphomas
- Fungal infections, especially other atypical Mycobacteria or Nocardia
Laboratory
- Nonspecific laboratory findings include anemia, monocytosis, thrombocytosis, hypergammaglobulinemia, SIADH and sterile pyuria
Drugs that may alter lab results:
- BCG: false-positive skin test but unreliable and should not influence decision to treat LTBI
- Steroids: false-negative skin test
Disorders that may alter lab results: False-negative skin test: Recent viral infections, new (<10 weeks) infection, severe malnutrition, HIV, anergy, age < 6 months, overwhelming TB
Pathological Findings
- Granulomas with foci of caseating necrosis surrounded by epithelioid histiocytes and giant cells, in turn surrounded by lymphocytes
- AFB stains positive
Special Tests
- Persons with TB should be tested for HIV; if positive, get CD4 count
- Baseline liver enzymes, bilirubin, creatinine, CBC with platelet count. If using ethambutol, baseline visual acuity and color discrimination. Test for hepatitis B and C if high risk.
- If extrapulmonary suspected, urine, CSF, bone marrow and liver biopsy for culture
Imaging
- CXR with primary disease: may show infiltrate with or without effusion atelectasis or adenopathy
- With recrudescent TB: cavitary lesions and upper lobe disease with hilar adenopathy common. Diffuse miliary pattern possible with appearance of “millet seeds”.
- HIV: atypical findings with primary infection — right upper lobe atelectasis
- CXR useful to rule out TB in asymptomatic infected persons
- CT chest — good sensitivity
Diagnostic Procedures
- PPD: 5 units (0.1 cc) intermediate strength intradermal volar forearm. Measure induration at 48-72 hrs.
- PPD positive if induration:
- > 5 mm and HIV infection (or suspected), immunosuppressed, recent close TB contact, clinical evidence of active or old disease on chest x-ray
- > 10 mm and age < 4 yrs or other risk factors – > 15 mm and age > 4 yrs and no risk factors
- PPD negative if induration:
- < 5 mm on initial test and, if indicated, on second test. Utilize 2-step test if patient has had no recent PPD, age > 55 years, nursing home resident, prison inmate, or healthcare worker (administer a second intradermal test 1 -3 weeks after initial test; measure and interpret as usual)
- For suspected pulmonary TB, obtain at least 3 morning sputum samples for AFB stain and culture — use aerosol induction, gastric aspirate (children) or bronchoalveolar lavage if needed
- AFB stain can give a presumptive diagnosis
- Culture confirms diagnosis; 4-6 weeks on solid media or2weeksonBACTEC broth system
- Direct nucleic acid amplification approved if AFB stain positive and < 7 days of antiTB treatment, provides rapid accurate detection, but expensive
- Culture and sensitivity guide treatment
Treatment (Medical Therapy)
Appropriate Health Care
- For active disease, treatment in the initial 2 month phase usually includes INH, RIF, PZA, EMB (for alternatives, see treatment algorithms). Two drugs are used in the continuation phase for 4-7 months, usually INH/RIF with choices based on clinical criteria.
- Treatment adherence plans using directly observed treatment or DOT (5 days/week) have the highest completion rates. DOT must be used for non-daily regimens, children, HIV, drug abuse, relapse or adherence not assured.
- For active TB and HIV+, note special precautions
- For inactive pulmonary TB on chest x-ray, use INH for 9 months
General Measures
Prescribing physician is responsible for treatment completion determined by total number doses taken, not just duration
Surgical Measures
For extra pulmonary complications (spinal cord compression, constric-tive pericarditis)
Activity
- As tolerated. Respiratory isolation for infectious pulmonary TB until clinical response and 3 ABF smears are negative.
- Children without cough and negative sputum smears: no isolation required after treatment started
Diet
Regular. Consider pyridoxine supplement.
Patient Education
- Teach pathogenesis, emphasize importance of drug therapy, warn of effects and/or interactions, and find contacts
- Inform local health department
Medications (Drugs, Medicines)
Drug(s) of Choice
Isoniazid (INH) — scored tabs 50/100/300 mg, syrup 10 mg/mL, or aqueous solution 100 mg/mL
- Daily dose: adult 300 mg; pediatric 10-15 mg/kg (maximum 300 mg)
- twice weekly: adult 15 mg/kg; pediatric 20-30 mg/kg (maximum 900 mg)
- Weekly: adult 15 mg/kg (maximum 900 mg)
- Consider adding pyridoxine 10-50 mg/day
Rifampin (RIF) capsules (150/300 mg, powder for oral suspension, or IV aqueous
- Daily dose: adult 600 mg; pediatric dose 10-20 mg/kg (maximum 600 mg)
- twice weekly: adult 600 mg; pediatric 10-20 mg/kg (maximum 600 mg)
Pyrazinamide (PZA), scored 500 mg
- Daily dose: adult 15-25 mg/kg (maximum 2 gm); pediatric 15-30 mg/kg (maximum 2 gm)
- Twice weekly: adult 50 mg/kg; pediatric 50 mg/kg (maximum 4 gm)
Rifabutin (Mycobutin) capsules 150 mg (pediatric not approved)
- Daily dose: adult 300 mg
- Twice weekly: adult 300 mg
Rifapentine (Priftine) tablet 150 mg (pediatric not approved); must be given with other medications
- Weekly dose: adult 600 mg (may be used in continuation phase for HIV negative, noncavitary TB, and negative sputum at second month)
Ethambutol (EMB) — tablets 100/400 mg bacteriostatic
- Daily dose: 15-20 mg/kg, with maximum of 1.6 gm
- Twice weekly: 50 mg/kg, with maximum of 4 gm
Contraindications:
- RIF: avoid if patient taking antiretrovirals
- Ethambutol: because of optic neuritis, avoid ethambutol unless patient old enough to cooperate for visual acuity and color testing.
Precautions:
- INH, RIF or PZA may cause hepatitis
- Follow liver function if the patient has history of liver dysfunction or new signs develop
- RIF — colors urine, tears and secretions orange. Can permanently stain contact lenses.
- INH — peripheral neuritis and hypersensitivity possible. Consider pyridoxine.
- PZA — may increase uric acid
- EMB — may cause optic neuritis; follow monthly vision and color tests
Significant possible interactions: Rifamycins alter the level of phenytoin, antivirals and other drugs metabolized by the liver and may inactivate birth control pills (recommend a barrier method). Monitor and adjust doses as needed.
Alternative Drugs
- Steroids — use only with concurrent anti-TB therapy. Recommended for meningitis or pericarditis.
- Other antituberculous drugs, especially quinolones, may be useful for multidrug resistant TB (MDRTB)
- Combination tablets enhance adherence
- Streptomycin (caution: ototoxicity and nephrotoxic; don’t use in pregnancy)
Patient Monitoring
- Assess monthly for treatment adherence and adverse effects
- Check liver enzymes if symptomatic, HIV positive, chronic liver disease, alcohol use, pregnant or postpartum, and modify drugs if needed
- During TB therapy — obtain sputum culture monthly until two consecutive specimens are negative
- If culture positive after 2 months of therapy, reassess drug sensitivity and initiate DOT
- CXR at 3 months
Prevention / Avoidance
- Identify and treat contagious persons. Notify public health department and hospital infection control if admitted
- Inpatient — use personal sealed respirators, negative pressure ventilation, ultraviolet
- Ambulatory patients use mask and tissues
- Not infectious if: favorable clinical response after 2-3 weeks of therapy and 3 AFB smears are negative.
Possible Complications
- Cavitary lesions can be secondarily infected
- Spread to susceptible persons of all ages
- Drug resistance — suspect if immigrant, drug resistant source or noncompliant
Expected Course / Prognosis
Generally few complications and full resolution if drugs taken for full course as prescribed
Miscellaneous
Associated Conditions
HIV infection (emphasize DOT; most recommendations remain the same). With HIV infection, delay initiation of antiretro-viral therapy 4-8 weeks after starting antituberculosis therapy.
Age-Related Factors
Pediatric:
- Emphasize DOT
- Caution with ethambutol
- Children on medication may attend school
- Disseminated TB more common in infants; prompt treatment with 4 drugs if TB suspected
- Congenital infection may occur with miliary TB of maternal bacillemia, endometritis or amniotic aspiration. If suspected, get PPD, CXR, LP, culture placenta and infant, then start treatment promptly
- Protocol for newborn with mother/household contact with infection or disease
- If mother or household contact has LTBI: skin test all household members and treat any with positive PPD
- Contact has abnormal CXR: separate infant until infectious status known; if not contagious, monitor infant PPD
- Mother with disease and possibly contagious: evaluate infant for congenital TB and test for HIV; separate newborn until member is noninfectious
- If congenital TB suspected, treat as above
- If no congenital disease, start INH and repeat PPD after 8-12 weeks.: If positive, reassess infant and finish 6 months INH. If PPD is negative, and source is noninfectious, stop INH and monitor infant.
- Consider BCG
Geriatric:
- Symptoms may be more subtle and may be attributed to associated conditions or to aging
- Side effects of INH more pronounced
Pregnancy
- Treat active TB in pregnant woman with INH, rifampin and ethambutol; add pyridoxine
- Avoid streptomycin
- Use PZA with caution
- Breast-feeding okay while taking TB drugs
Synonyms
Consumption
International Classification of Diseases
011.90 Pulmonary tuberculosis, unspecified
See Also
Tuberculosis, latent Tuberculosis, CNS
Other Notes
BCG vaccine, live attenuated Mycobacterium bovis
- 50% efficacy for pediatric and adult pulmonary TB
- In USA, consider BCG for children with negative PPD and HI V tests with unavoidable high risk and for health care workers at high risk for drug resistant infection
- Abscess, ulceration and regional lymphadenitis occur in 1-2%, osteitis and fatal infection can occur in immunosuppressed
- Used more commonly in developing countries to prevent complications of TB
Abbreviations
PPD = purified protein derivative
BCG = Bacillus Calmette-Guerin
DOT = directly observed treatment
LTBI = latent tuberculosis infection




