General Considerations
Epidemiology
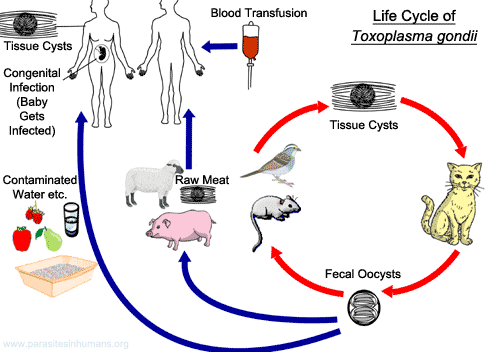
Toxoplasma gondii infection, or toxoplasmosis, is a zoonosis (the definitive hosts are members of the cat family). The two most common routes of infection in humans are by oral ingestion of the parasite and by transplacental (congenital) transmission to the fetus. Ingestion of undercooked or raw meat that contains cysts or of water or food contaminated with oocysts results in acute infection.
In humans, the prevalence of toxoplasmosis increases with age. There are also considerable geographic differences in prevalence rates (eg, 10% in Palo Alto, CA; 15% in Boston, MA; 30% in Birmingham, AL; 70% in France; = 90% in El Salvador). Differences in the epidemiology of T gondii infection in various geographic locales and between population groups within the same locale may be explained by differences in exposure to the organism. Occasionally, outbreaks occur within families or certain populations. The possibility of an outbreak should always be suspected with every case of recently acquired acute infection.
The incidence of congenital toxoplasmosis is directly correlated with three factors: (1) the prevalence of primary infection among women during pregnancy, (2) the gestational age at which a pregnant woman acquires the infection, and (3) the types of public health programs available for prevention, detection, and treatment of the infection during pregnancy. Although screening for Toxoplasma infection is compulsory during pregnancy in some countries such as Austria and France, routine serological screening is not performed in the United States. Without any therapeutic intervention, the incidence of congenital toxoplasmosis is ~ 15% for a fetus whose mother becomes infected during the first trimester, 30% during the second trimester, and 60% during the third trimester. Spiramycin decreases the incidence of fetal infection by ~ 60%. It has been reported that, if maternal infection is acquired during the first 2 weeks of gestation and spiramycin is administered for the entire pregnancy, the incidence of fetal infection is negligible.
As an opportunistic pathogen in HIV-infected persons, T gondii has had a major impact on public health. The incidence of toxoplasmosis in an HIV-infected population is directly correlated with four factors: (1) the prevalence of anti-Toxoplasma antibodies, (2) the degree of immunosuppression as estimated by the CD4 cell count, (3) the frequency with which effective prophylactic regimens against Toxoplasma reactivation are used, and (4) the frequency with which highly active antiretroviral therapy is used. Of individuals seropositive for both HIV and Toxoplasma with CD4 counts of < 100 cells/mm3, 30%-50% will develop toxoplasmic encephalitis (TE) if prophylaxis is not used. Genetic factors may also play a role in predisposition of AIDS patients for this disease, based on findings from a murine model of TE and the observation that not all HIV-infected patients with positive T gondii serology develop TE. Human lymphocyte antigen DQ3 appears to be a genetic marker of susceptibility to development of TE in AIDS patients, and DQ1 may be a marker of resistance.
Even before the emergence of AIDS, TE had been recognized as a major cause of morbidity and mortality among non-HIV-immunosuppressed patients, especially in those whose underlying disease or therapy caused a deficiency in T-cell-mediated immunity (eg, Hodgkin’s disease and heart, lung, kidney, and bone marrow transplantation).
Microbiology
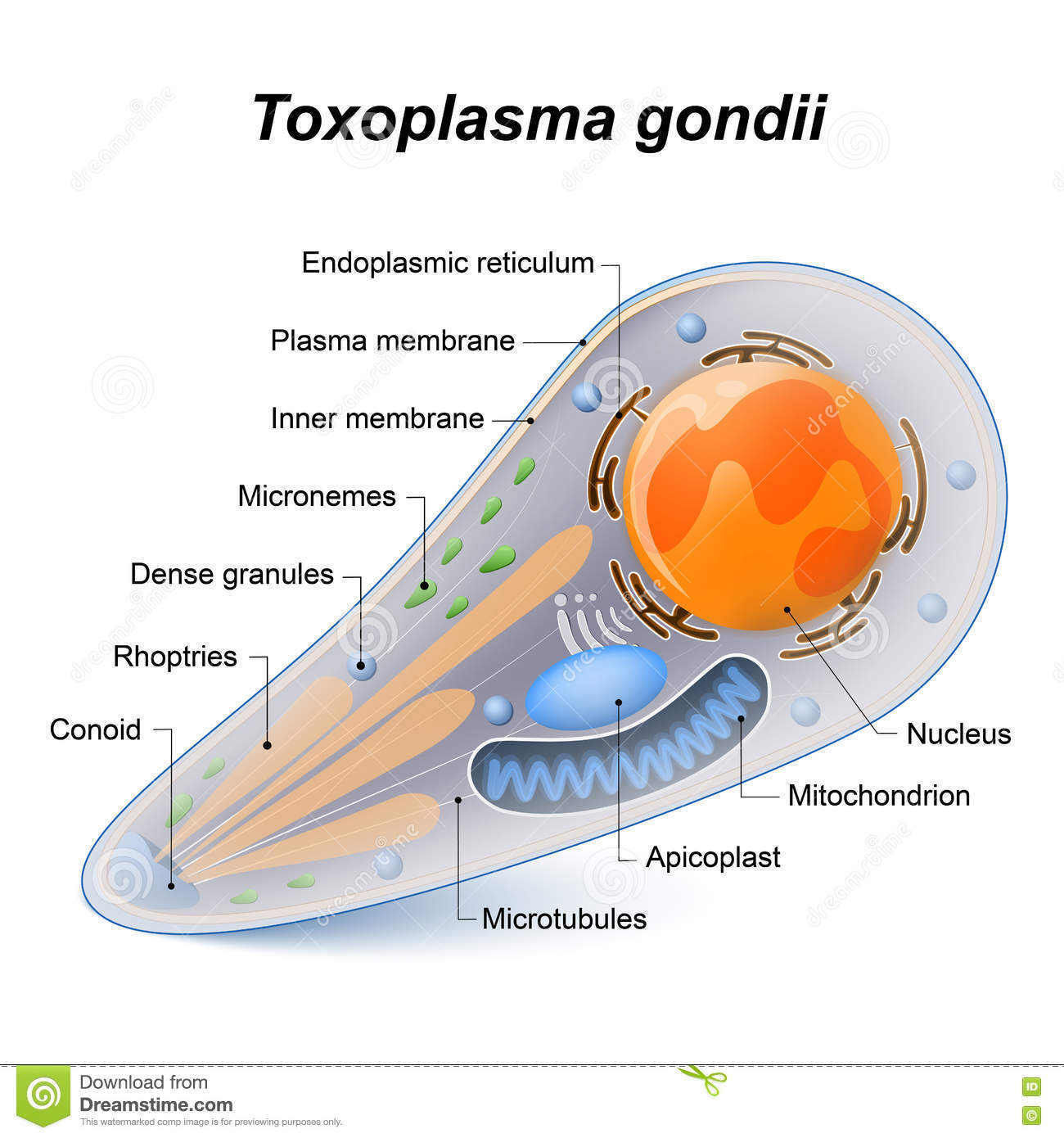
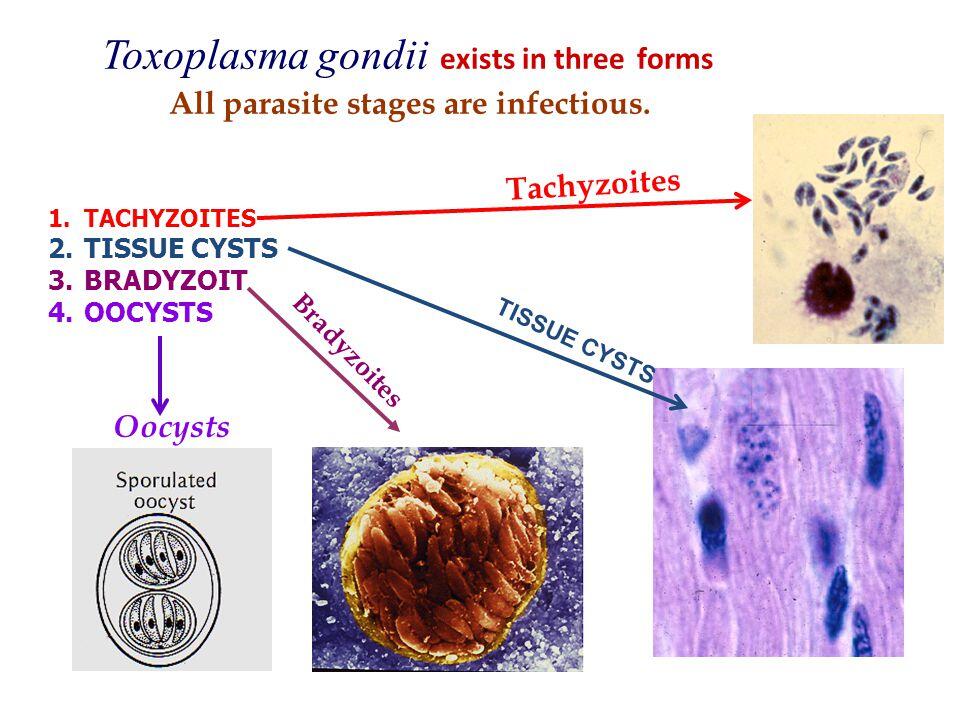
T gondii is an obligate intracellular coccidian protozoan that exists in three forms: the oocyst (which releases sporozoites), the tachyzoite, and the tissue cyst (which contains and may release bradyzoites). The parasite undergoes two cycles, an enteroepithelial sexual cycle in the small bowel of members of the cat family and an extraintestinal asexual cycle in cats as well as in all other infected animals, including humans. Cats shed oocysts after they ingest any of the three forms of the parasite. Humans usually become infected by ingestion of tissue cysts (in meat) or oocysts (in cat feces); the outer walls of both are disrupted by enzymatic degradation, and the parasites are liberated into the intestinal lumen. They become tachyzoites and spread to virtually all cells and tissues of the body.
- Oocyst. Oocysts are formed in the small bowel of members of the cat family and are excreted in their feces for 7-20 days. They are highly resistant to conditions found within the external environment. As many as 10 million oocysts may be shed in a single day and will become infectious (by sporulation) in 1-21 days, depending on temperature and availability of oxygen.
- Tachyzoite. Tachyzoites are crescent or oval shaped and measure 2-4 um wide by 4-8 um long. They require an intracellular habitat to survive and multiply despite having their own Golgi apparatus, ribosomes, and mitochondria. Tachyzoites penetrate host cells by an active process involving the components of an “apical complex” (hence the term apicomplexan). They reside and multiply within an intracellular parasitophorous vacuole whose composition (eg, acidity) is dictated in large part by the parasite. In the laboratory, tachyzoites are propagated in the peritoneum of mice and in tissue-cultured mammalian cells. The presence of tachyzoites in human fluids or tissues is the hallmark of acute infection.
- Tissue cyst. After cell entry and replication of the tachyzoite form, encystation and formation of tissue cysts may occur. The precise conditions that promote cyst formation are not known. The tissue cyst is formed within a host cell and may vary in size from those containing only a few organisms (bradyzoites) to those = 200 um in diameter containing several thousand bradyzoites. Tissue cysts stain well with periodic acid-Schiff reagent, Wright-Giemsa, Gomori-methenamine silver, and immunoperoxidase stains. The cysts are spherical when found in the brain and conform to the shape of muscle fibers when in heart and skeletal muscle tissue. The most common sites of latent infection are the central nervous system (CNS); eye; and skeletal, smooth, and heart muscles. Because of this persistence in tissues, demonstration of cysts in histologic sections does not necessarily mean that the infection was recently acquired or that it is clinically relevant.
- Stage conversion. Tachyzoites and bradyzoites differ phenotypically. Tachyzoites multiply rapidly and synchronously, forming rosettes, thereby lysing the cell, whereas the more slowly replicating bradyzoites form tissue cysts. Major differences in energy metabolism and in antigenic structure of tachyzoites and bradyzoites reflect the expression of stage-specific pathways and molecules that promote parasite survival in diverse environments and under diverse conditions within the host.
Pathogenesis
T gondii multiplies inside cells at the site of invasion (the gastrointestinal tract appears to be the major route for and the initial site of infection in nature). After host cell disruption, parasites invade adjacent cells from which they spread throughout the body via lymphatics and the bloodstream. Humoral immunity and cellular immunity appear to curtail successfully the parasitemic phase; only those parasites protected by an intracellular habitat or within tissue cysts survive. An effective immune response is also responsible for a significant early reduction in the number of T gondii in all tissues. Thereafter, tachyzoites are rarely demonstrated in tissues.
The tissue cyst form is responsible for residual infection and persists primarily in brain, skeletal, and heart muscle, and in the eye. Whereas toxoplasmosis in severely immunodeficient individuals may be caused by primary infection, it most often is the result of recrudescence of a latent infection.
The histopathologic changes of toxoplasmic lymphadenitis are frequently diagnostic in immunocompetent individuals. There is a characteristic triad of findings: a reactive follicular hyperplasia, irregular clusters of epithelioid histiocytes encroaching on and blurring the margins of the germinal centers, and focal distension of sinuses with monocytoid cells.
Ocular involvement in immunocompetent patients produces acute retinochoroiditis characterized by necrosis and severe inflammation. Granulomatous inflammation of the choroid is secondary to the necrotizing retinitis.
Involvement of the CNS is characterized by multiple enlarging foci of necrosis and microglial nodules. Necrosis is the most salient feature of the disease because of vascular involvement. The presence of multiple brain abscesses is the most typical feature of TE in severely immunodeficient patients and is particularly characteristic in patients with AIDS. At autopsy in most AIDS patients with TE, cerebral hemispheres are involved, with a peculiar predilection for the basal ganglia. Pulmonary toxoplasmosis in the immunodeficient patient may present as interstitial pneumonitis, necrotizing pneumonitis, consolidation, and/or pleural effusion. Chorioretinitis in AIDS patients is characterized by segmental panophthalmitis and areas of coagulative necrosis associated with tissue cysts and tachyzoites.
Immunity to T gondii
After disease in the immunocompetent host, immunity against T gondii is lifelong. Cellular immunity appears to be more important than humoral immunity in defense of the brain. A well-orchestrated interaction between CD4 and CD8 T lymphocytes; lymphokine-activated killer, natural killer, and ?d T cells; and cytokines such as interferon-?, tumor necrosis factor-a, interleukin-1 (IL-1), IL-2, IL-4, IL-6, IL-7, IL-10, IL-12, and IL-15 appears to determine the outcome of the parasite-human host interaction. Nitric oxide may have a tissue-specific protective role.
Toxoplasma Gondii: Clinical Findings Clinical Findings
Differential Diagnosis
The differential diagnosis of toxoplasmic lymphadenitis includes lymphoma, Epstein-Barr virus-associated infectious mononucleosis, CMV “mononucleosis,” cat scratch disease, sarcoidosis, tuberculosis, tularemia, and metastatic carcinoma. For toxoplasmic encephalitis, the differential diagnosis includes primary CNS lymphoma, JC virus-associated progressive multifocal leukoencephalopathy, CMV ventriculitis, tuberculoma, cryptococoma, and bacterial or nocardial brain abscess. None of the signs described in newborns with congenital disease are pathognomonic for toxoplasmosis, and all of them may be mimicked by congenital infection with other pathogens, including CMV, Treponema pallidum, herpes simplex virus, and rubella virus.
Complications
In rare instances, toxoplasmosis causes myocarditis, polymyositis, pneumonitis, hepatitis, or encephalitis in healthy individuals. Early maternal infections sometimes result in death of the fetus in utero and spontaneous abortion.
Prevention & Control
Prevention of the primary infection is of paramount importance in pregnant women and immunodeficient patients who are seronegative (Box 6). Tissue cysts in meat are rendered noninfectious by heating the meat to 66 °C (meat should be cooked to “well done” with no pink meat visible in the center), by smoking or curing it, or by freezing it to -20 °C (which is not achieved in most home freezers). Hands should be washed meticulously after handling raw meat or vegetables; eggs should not be eaten raw, and unpasteurized milk (particularly milk from goats) should be avoided. Flies and cockroaches should be controlled. Areas contaminated with cat feces should be avoided entirely. Disposable gloves should be worn while disposing of cat litter (if this task cannot be avoided altogether), working in the garden, or cleaning a child’s sandbox. Oocysts are killed if the cat litter container is soaked in nearly boiling water for 5 min. If the litter container is cleaned every day, oocysts will not have a chance to sporulate.
There is no vaccine currently available for prevention of toxoplasmosis in humans; primary prophylaxis against toxoplasmosis in patients with AIDS who are at high risk of developing TE has been shown to be effective. Primary prophylaxis is recommended for seropositive patients whose CD4 count has been < 100 cells/mm3 (some experts use a cutoff of < 200 cells/mm3), regardless of the HIV RNA viral load. Trimethoprim-sulfamethoxazole and dapsone plus pyrimethamine have been reported to be effective regimens in preventing the first episode of TE (Box 7). Pyrimethamine has been used post-transplantation for primary prophylaxis in seronegative heart transplant recipients whose donors are seropositive (Box 7).
Table 1. Laboratory tests for the diagnosis of toxoplasmosis.
- Serology (IgG) is useful to establish whether the patient has been exposed to T gondii.1 It can also indicate whether the infection is acute or chronic.2,3
- Histology (hematoxylin and eosin, immunoperoxidase, Wright-Giemsa and periodic acid-Schiff stains). The presence of tachyzoites is diagnostic of acute infection. Solitary cysts do not necessarily indicate acute or reactivated disease.
- Isolation of the parasite from any tissue by mouse or tissue culture inoculation is diagonostic.2
- PCR-based detection of DNA in amniotic fluid, CSF, ocular fluids, bronchoalveolar lavage, peripheral blood, and urine is diagnostic.2
- Radiographic studies are helpful when suspecting CNS toxoplasmosis in the fetus or newborn (ultrasound or CT) and immunocompromised patients (CT or MRI).
- In most cases, ocular toxoplasmosis is a clinical diagnosis.
- Confirmatory serological tests include the Sabin-Feldman dye test for IgG, IgM ELISA, IgA ELISA, differential agglutination test, and IgE ELISA.
- Consultation with a reference laboratory is strongly recommended.
- Serological diagnosis may not be useful in immunocompromised individuals.
Table 2. Interpretation of Toxoplasma serology in pregnant women.1
IgG result
IgM result
Interpretation and
Recommendation
Negative
Negative
No serologic evidence of infection with T gondii
Negative
Equivocal or positive
Possible acute infection or false positive IgM. Send sample to reference laboratory
Equivocal for IgG in a different assay
Negative
Indeterminate; obtain a new specimen for testing or retest
Equivocal testing
Equivocal
Indeterminate; obtain a new specimen for both IgG and IgM
Equivocal laboratory
Positive
Possible acute infection. Send sample to reference
Positive
Negative
Infected with T gondii for > 6 months
Positive
Equivocal or positive
Possible acute infection. Send sample to reference laboratory
- Modified from US Food and Drug Administration Public Health Advisory: Limitations of Toxoplasma IgM Commercial Test Kits.
BOX 1. Clinical Syndromes Associated with Toxoplasmosis1
Patient
Syndromes
Immunocompetent
- Asymptomatic
- 90% of acute infection goes unrecognized
- Lymphadenitis
- Regional or generalized lymphadenopathy
- Chorioretinitis
- Intensely white focal retinal lesions with overlying vitritis, with or without associated scars; may result from reactivation of congenital or postnatally acquired disease or from recently acquired acute disease
- Myocarditis
- Arrythmias, pericarditis, heart failure
- Polymyositis
- Patients with acute toxoplasmosis have developed polymyositis/dermatomyositis-like syndromes
- Systemic
- Low-grade fever, general malaise, headache, sore throat, myalgia
- Disseminated disease is extremely rare; may present with fever, pneumonitis, hepatitis, or, possibly, encephalitis
Immunocompromised
- Encephalitis
- Focal or nonfocal neurological symptoms and/or mental status changes; usually occurs in the setting of advanced T-cell-mediated immunity impairment
- Chorioretinitis
- Can present atypically and/or with significant retinal necrosis
- Myelopathy
- Cervical, thoracic, or lumbar
- Pneumonitis
- Interstitial infiltrates
- Systemic
- Fever, multiorgan involvement, acute respiratory failure, and septic shocklike syndrome
Pregnant
- Asymptomatic
- 90% of acute infection goes unrecognized
- Lymphadenitis
- Regional or generalized lymphadenopathy
Fetus
- Neurologic disease
- Ultrasound may be normal or reveal ventricular dilatation, intracranial calcifications
- Generalized disease
- Ultrasound may be normal or reveal increased placental thickness, hepatomegaly, ascites
Newborn
- Asymptomatic
- 85% of newborns with congenital disease appear normal at birth
- Neurologic disease
- Seizures, chorioretinitis, abnormal neurological exam, hydrocephalus, cerebral calcifications
- Generalized disease
- Fever, hepatosplenomegaly, lymphadenopathy, jaundice, thrombocytopenia, anemia
- Syndromes are not mutually exclusive. Patients may present simultaneously or sequentially with two or more syndromes (ie, an otherwise immunocompetent patient may have lymphadenitis and chorioretinitis, or a newborn may present with hydrocephalus, cerebral calcifications, and thrombocytopenia).
BOX 2. Treatment of Toxoplasmosis in Immunocompetent Patients
Syndrome
Drug
Children
Adults
Lymphadenitis
None
No therapy
No therapy
Chorioretinitis (active), myocarditis, polymyositis, systemic2
- Pyrimethamine PLUS
- Loading dose: 2 mg/kg/d (maximum, 50 mg) for 2 days, then maintenance, 1 mg/kg/d (maximum 25 mg)
- Loading dose: 75-100 mg over 24 h, followed by 25 to 50 mg/d
- Sulfadiazine3 PLUS
- Loading dose: 75 mg/kg, then maintenance, 50 mg/kg every 12 h (maximum 4 g/d)
- Loading dose: 2-4 g initially, followed by 1 g four times per day
- Folinic acid
- 5-20 mg, 3 times weekly
- 5-10 mg/d
- Corticosteroids (if indicated)
- 1 mg/kg/d in 2 divided doses
- Dosing varies with clinical setting
- Treatment may be indicated if accompanying symptoms are severe or persistent.
BOX 3. Treatment of Toxoplasmosis in Pregnant Women
Syndrome
Drug
Dosages
Acute infection acquired during gestation
- Spiramycin (should be continued for the entire pregnancy even if amniotic fluid PCR is negative)
3 g/d
Amniotic fluid PCR-positive result at 18 weeks of gestation or later
- Pyrimethamine PLUS sulfadiazine PLUS folinic acid starting after 18th wk of gestation
- Same doses as for immunocompetent patient
- The role of other regimens, including drugs such as atovaquone, clarithromycin, azithromycin, trimethoprim/sulfamethoxazole, or dapsone, has not been well established.
- Clindamycin (300 mg by mouth every 6 h for a minimum of 3 weeks) is an alternative in patients allergic to sulfonamides.
BOX 4. Treatment of Toxoplasmosis in Newborns
Drug
Dosages
Pyrimethamine
PLUS
- Loading dose: 2 mg/kg/d (maximum, 50 mg) or 2 d, then 1 mg/kg/d for 2 or 6 mo. After 2 or 6 mo, 1 mg/kg/d every Monday, Wednesday, and Friday
Sulfadiazine1 PLUS
- 50 mg/kg every 12 h
Folinic acid
- 5-20 mg 3 times weekly
Corticosteroids (if indicated)
1 mg/kg/d in 2 divided doses
- Clindamycin is an alternative in patients allergic to sulfonamides.
BOX 5. Treatment of Toxoplasmosis in Immunocompromised Patients
Drug
Children
Adults
Pyrimethamine PLUS
- Loading dose: 2 mg/kg/d (maximum, 50 mg) for 2 days, then maintenance, 1 mg/kg/d (maximum 25 mg)
- Loading dose: 200 mg over 24 h, followed by 50-75 mg/d
Sulfadiazine1 PLUS
- Loading dose: 75 mg/kg, then maintenance, 50 mg/kg every 12 h (maximum 4 g/d)
- Loading dose: 2-4 g initially, followed by 1-1.5 g four times per day
Folinic acid
- 5-20 mg 3 times weekly
- 5-10 mg/d (= 50 mg/d)
- Clindamycin (300 mg by mouth every 6 h for a minimum of 3 weeks) is an alternative in patients allergic to sulfonamides.
BOX 6. Prevention of Primary T gondii Infection1
Infectious Form
Preventive Measure
Tissue cyst (meat)
- Wash hands thoroughly after contact with raw meat
- Avoid mucous membrane contact when handling raw meat
- Wash kitchen surfaces and utensils that have come in contact with raw meat
- Cook meat well done (meat that is cured in brine may be infectious)
- Avoid ingestion of dried meat
- Refrain from skinning animals
Oocyst (cat feces)
- Wash fruits and vegetables before consumption
- Avoid contact with materials potentially contaminated with cat feces
- Wear gloves when gardening or handling cat litter
- Disinfect cat litter with near boiling water for 5 min before handling
BOX 7. Primary Prophylaxis in Immunodeficient Patients
Patient
Regimen
AIDS patients at high risk of developing TE
- Trimethoprim/sulfameth-oxazole (either 160 mg/800 mg or 80 mg/400 mg/d) or dapsone (50 mg/d) plus pyrimethamine (50 mg/week)
Heart transplant patients whose donors are seropositive
- Pyrimethamine (25 mg by mouth once daily for 6 weeks, post-transplant)
More Information:
https://www.ncbi.nlm.nih.gov/books/NBK7752/
https://www.cdc.gov/parasites/toxoplasmosis/gen_info/faqs.html