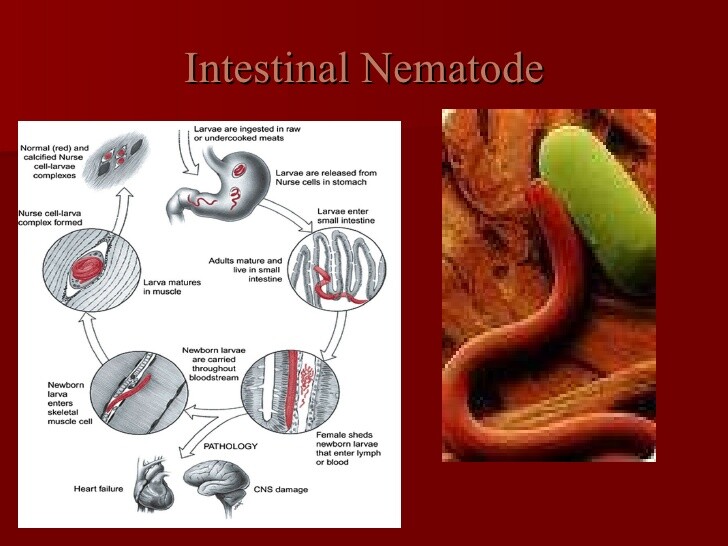
ASCARIASIS
Worldwide, more than 1 billion people are infested with Ascaris lumbricoides, the causative agent of ascariasis or roundworm. More than 4 million people are estimated to be infected in the United States. Infection occurs predominately in the southeastern states and more commonly in younger children, and it is associated with lower socioeconomic status.
The organism is acquired through ingestion of embryonic forms of the worm, which are found in fecally contaminated soil. After ingestion, the embryonic eggs hatch in the small intestine, and the larvae undergo a tissue migration phase. During the migration, the larvae penetrate the intestinal wall and travel intravenously to the pulmonary alveoli. In the lungs, the organisms provoke a cough, are swallowed by the host, and subsequently mature into the adult worm in the small intestine. A single adult female ascarid may produce 200,000 ova daily, which are shed in the feces.
Clinical Findings
The majority of ascarid infections are asymptomatic. During larval migration, eosinophilic pneumonia with mild fever, cough, wheezing, pulmonary infiltrates, and peripheral eosinophilia may be seen. Heavier worm loads may result in intestinal obstruction or symptoms caused by migration of the adult worm outside of the small intestine, most commonly into the common bile duct, causing biliary obstruction and associated complications. Rarely, adult worms may be expelled from the anus, nose, or mouth.
Differential Diagnosis
During tissue and pulmonary larval migration, other causes of pulmonary infiltrates with eosinophilia, including hookworm and strongyloides infection, as well as Loffler’s syndrome, asthma, and allergic bronchopulmonary aspergillosis, should be considered. Heavy intestinal infection may cause obstruction that mimics other mechanical causes of bowel obstruction. Migration into the biliary system or appendix may be confused with acute cholecystitis, appendicitis, acute abdomen, or biliary obstruction caused by other more common causes.
Treatment
All patients with ascariasis should be treated, even if asymptomatic, to prevent biliary migration and obstruction (Box 2). Ascarids should be treated first in mixed parasitic infections, and they should be treated before general anesthesia because of the risk of inducing migration of hypermotile worms. In some cases, endoscopic removal of worms may be indicated. Stools should be reexamined 2 weeks after therapy and treatment repeated as necessary.
Prognosis
Prognosis is generally excellent, although reinfection is possible. In rare cases, obstruction of the small intestine by a mass of worms may cause an acute abdominal syndrome. In addition, obstruction of the common bile duct may cause acute biliary colic.
Prevention
Roundworm infection can be prevented by avoiding ingestion of fecally contaminated soil. Measures to accomplish this include hygienic disposal of fecal waste, avoidance of the use of night soil and proper washing of foods contaminated by soil, hand washing, and avoidance of pica.
ENTEROBIASIS
Also known as pinworm, infection by Enterobius vermicularis is the most common helminth infection in the United States. Enterobiasis is typically found in clusters of individuals living in close proximity, such as families or institutionalized groups. It is particularly common in school-age children. Adult females migrate nocturnally to the perianal areas, where eggs are deposited and subsequently distributed to fingers, fingernails, bedding, nightclothes, and other areas. Ingestion of the embryonated eggs results in development of intestinal adult worms in 1-2 months.
Clinical & Laboratory Findings
Many infections are asymptomatic. In symptomatic patients, nocturnal anal pruritus and interrupted sleep are typical. Laboratory tests are normal; eosinophilia is not seen with enterobiasis. Although adult worms that resemble small threads may be seen with the naked eye, diagnosis is usually made by documenting eggs in the perianal area in the early morning, before bathing or defecation. This can be done by pressing cellophane tape in the perianal area and examining the tape under the microscope or by using a commercial collection system such as the Swube (Becton Dickinson). Stool examination for eggs is usually not helpful.
Differential Diagnosis
Enterobiasis should be distinguished from other causes of perirectal irritation, including pruritis ani, rectal fissures, moniliasis, hemorrhoids, and strongyloidiasis, among other conditions.
Treatment
Treatment suggestions are given in Box 2.
Prognosis
Prognosis is excellent, although reinfection is common in the setting of continued exposure.
Prevention
Reinfection is common in households with an infected person; examination for asymptomatic carriers and simultaneous treatment of all infected household members may be required. Household members should practice hand washing before meals and after defecation and should launder bedding and bedclothes to eliminate environmental eggs.
ANCYLOSTOMIASIS & NECATORIASIS
Hookworm infestation is caused by Ancylostoma duodenale or Necator americanus. After hookworm eggs are passed in stool, the larvae hatch and mature in soil, where they become infective after 1 wk. Human infection occurs after direct penetration by larvae of the host’s skin, usually through the feet. The hookworm larvae then enter venules and are carried to the lungs, where they penetrate into alveoli. From the alveoli, the larvae migrate to the trachea. They induce cough and are swallowed by the host. The larvae mature into adult worms in the small intestine. Hookworms attach to intestinal mucosa by means of teeth and a well-developed mouth, and they feed on blood and nutrients sucked from the host. Humans are the only known hosts.
Clinical & Laboratory Findings
The initial allergic reaction to larval skin penetration and migration is known as “ground itch,” and is manifested by intense pruritus and vesicular or maculopapular dermatitis. Patients may experience cough, wheezing, fever, and pulmonary infiltrates during pulmonary migration. Peripheral eosinophilia may be marked. During the intestinal phase, which may last several years, heavy worm burdens may result in protein malnutrition and iron deficiency anemia.
Differential Diagnosis
Early in infection, strongyloidiasis, cutaneous larva migrans, contact dermatitis, scabies, and other causes of pruritic dermatitis, especially of the extremities, should be considered. Later, other causes of eosinophilic pneumonia should be considered, including A lumbricoides and Strongyloides stercoralis infections, as well as Loffler’s syndrome. Chronic intestinal infestation, with nonspecific gastrointestinal symptoms, may mimic a multitude of gastrointestinal conditions and other causes of iron deficiency.
Treatment
Re-treatment at 2-wk intervals may be necessary to reduce the worm burden to low levels (see Box 2). Because light infections are usually asymptomatic, complete eradication may not be therapeutically necessary. In patients with iron deficiency, supplemental iron therapy (eg, ferrous sulfate, 200 mg 3 times daily for several months, followed by 200 mg daily until iron stores are repleted) may be necessary.
Prognosis
Prognosis with treatment is excellent.
STRONGYLOIDIASIS
Infection by S stercoralis (threadworm) is especially notable because the worm is parthenogenetic and larvae mature to an infective stage within the intestinal lumen. As a consequence, sequential generations of worms may persist in a single host over many years. Immunocompromise caused by organ transplantation, corticosteroid therapy, hematologic malignancies, or other conditions may result in massive autoinfection, termed the hyperinfection syndrome. Surprisingly, human immunodeficiency virus infection does not appear to increase susceptibility for hyperinfection.
Like other intestinal nematodes, the life cycle of S stercoralis is complex. The initial infection occurs through penetration of the skin by soil-borne free-living infectious larvae. The larvae ultimately reach the proximal intestine via blood-lung migration. Eggs from adult worms hatch in the intestine, producing larvae that may (i) reinfect the same host, (ii) pass to a new host directly via skin penetration, or (iii) give rise to soil-borne free-living adults that may, in turn, produce infectious larvae.
Clinical & Laboratory Findings
Many patients with chronic but low worm burden infections are asymptomatic or have irregular intestinal symptoms. During initial skin penetration, local skin irritation, pruritic dermatitis, urticaria, and serpiginous tracts (“larva currens”) may be seen. During pulmonary migration, symptoms and signs of infection are similar to those of other nematodes that travel through the lung; that is, dry cough, wheezing, low-grade fever, dyspnea, and hemoptysis. Symptoms of chronic intestinal infestation are varied and nonspecific, and they may include bloating, abdominal distension, dyspepsia, epigastric pain, pruritus ani, diarrhea, and flatulence. In immunocompromised patients, hyperinfection syndrome may be manifested by gastrointestinal ulceration, peritonitis, ileus, biliary obstruction, cholecystitis, or hepatic granulomas. Invasion of extraintestinal organs, including meningitis, central nervous system invasion, pericarditis or myocarditis, or pleuritis, may also occur. Gram-negative or polymicrobial bacteremia with sepsis may complicate hyperinfection syndrome.
Diagnosis of strongyloidiasis is made by examination of stool or duodenal aspirate for S stercoralis larvae. Larvae may be present in stool only intermittently. Eggs of S stercoralis are rarely seen in stool specimens.
Differential Diagnosis
The myriad of presentations and potential tissue sites of S stercoralis requires a high index of suspicion for diagnosis. Chronic intestinal symptoms may mimic dyspepsia, irritable-bowel syndrome, inflammatory-bowel disease, malabsorption, sprue, giardial infection, or other causes of chronic or recurring diarrhea. Epigastric pain may resemble peptic ulcer disease. During tissue migration, eosinophilia, pulmonary infiltrates, wheezing, and cough may suggest nematode or ascarid infections as well as asthma, hypersensitivity pneumonitis, allergic bronchopulmonary aspergillosis, or Loffler’s syndrome. Hyperinfection syndrome may mimic sepsis or bacteremia caused by enteric organisms from other causes, such as aortoenteric fistula.
Treatment
Eradication is the goal of therapy (see Box 2). When immunosuppression can be anticipated, such as in patients being evaluated for organ transplantation, screening for S stercoralis and eradication should occur before immunosuppression.
Prognosis
In immunocompetent hosts, prognosis is good. Severe infection with multiple complications may occur in immunocompromised hosts with hyperinfection syndrome.
TRICHURIASIS
Trichuriasis or whipworm is caused by Trichuris trichiura. These small (30- to 50-mm-length) whiplike nematodes attach to the mucosa of the large intestine, especially the cecum; there is no extraintestinal phase. Infection occurs by ingestion of infective eggs from soil contaminated with feces; 2-4 wk of maturation in soil are required for the larvae within the eggs to become infective; thus, direct person-to-person transmission does not occur.
Clinical & Laboratory Findings
Mild to moderate worm burdens are usually asymptomatic. Heavy infections (> 30,000 eggs/g of feces) may be asymptomatic or cause nonspecific abdominal complaints, including abdominal cramping, bloating, distension, nausea, vomiting, flatulence, diarrhea, or tenesmus. Rectal prolapse and appendiceal obstruction with appendicitis are rare complications of strongyloidiasis. Eosinophilia is common; iron deficiency anemia may be seen with heavy infections that result in chronic occult blood loss.
Treatment
Treatment of symptomatic trichuriasis is outlined in Box 2.
Prognosis
Prognosis is excellent.