Essentials of Diagnosis
Epidemiologic factors: time spent in an endemic zone; poor housing conditions, eg, mud or thatched housing; exposure to reduviid insect vector
History and physical exam: Romana’s sign (swollen periorbital mucosal tissues after ocular inoculation); chagoma (skin nodule at the site of acute inoculation); in the chronic phase, congestive heart failure, dysphagia or regurgitation, and constipation
Laboratory exam:
- Acute Chagas’: trypomastigotes revealed by Giemsa smear of blood or buffy coat; culture of affected tissues, ie, the inoculation site; serologic enzyme immunoassay and enzyme-linked immunosorbent assay (ELISA); xenodiagnosis if available
- Chronic Chagas’: radiological studies show congestive heart failure, megacolon, or megaesophagus; ECG shows right bundle branch block, arrhythmias
General Considerations
Epidemiology
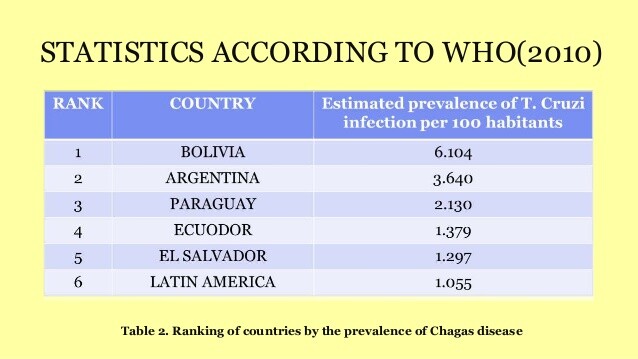
T cruzi is found only in the Western Hemisphere, where it ranges from the southern United States to Argentina. An estimated 16 million-18 million people in Latin America have chronic T cruzi infections and ~ 50,000 die of Chagas’ disease each year. In the United States, there has been concern about transmission of the organism via blood transfusion from unsuspected infected donors who are immigrants from endemic zones. Similar concerns arise for organ transplant recipients.
Microbiology
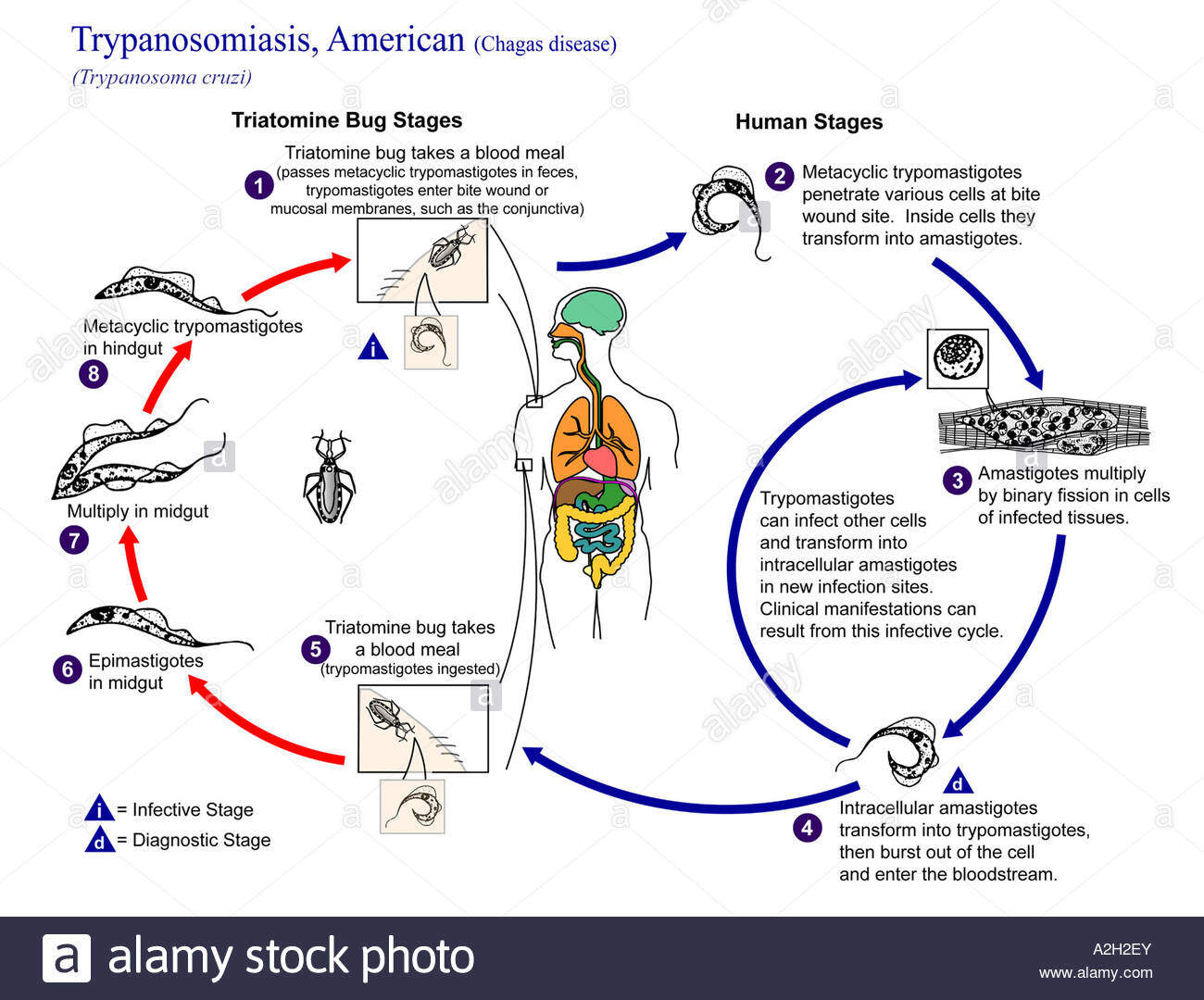
The life cycle of T cruzi involves an insect vector, the reduviid bug, and a mammalian reservoir. The insect vector, of which there are multiple species, is commonly known as an assassin bug because it preys on other insects; it is also called the kissing bug because it tends to bite the face. After taking a blood meal from an infected reservoir, T cruzi organisms multiply in the insect mid gut as epimastigotes and then develop into the infective form, the trypomastigote, in the insect hindgut. There are several nonhuman mammalian reservoirs that enable T cruzi to persist in nature, including peridomestic animals such as cats, dogs, and rats, as well as sylvatic animals such as opossums, raccoons, and armadillos.
Pathogenesis
When an infected reduviid bug takes a blood meal from a human, it defecates, leaving feces on the surface of the skin that is contaminated with the infective metacyclic stage of the trypanosomes. Trypanosomes proliferate at the site of inoculation and then pruritus at the bite wound causes T cruzi organisms to be rubbed into the wound or surrounding mucous membranes, introducing the organism to the bloodstream. In the bloodstream, they preferentially infect myocytes and neurons of the peripheral and central nervous system (CNS). After the amastigotes proliferate in the cytoplasm, they differentiate into trypanomastigotes. The cell subsequently ruptures, and the newly released trypanomastigotes invade local tissues and spread hematogenously. A mononuclear inflammatory response occurs. This intense inflammation leads to destruction of autonomic ganglia in the heart and gastrointestinal tract, and diffuse fibrosis and scarring occur in these organs.
Clinical Findings
In the acute phase of American trypanosomiasis, an indurated erythematous lesion occurs a few days after inoculation of T cruzi into the skin. This is called a chagoma. Periorbital swelling results when trypanosomes are inoculated into the conjunctival mucous membranes, and it is a classic sign of acute infection known as Romana’s sign. The patient experiences fever, hepatosplenomegaly, lymphadenopathy, transient skin rash, tender subcutaneous nodules (known as hematogenous chagomas), and nonpitting edema on the face or extremities. The acute phase is more commonly observed in children and is usually self-limited, lasting several weeks to months. Dissemination of organisms is common, regardless of whether chronic disease ultimately develops.
Chronic American trypanosomiasis is usually insidious. There may not be a history of documented acute disease. About 10-30% of infected patients develop chronic disease. These patients progress to have cardiac or gastrointestinal damage that results in clinical disease. Chronic infection may evolve over decades and most often involves the heart. Cardiac disease is manifested by biventricular hypertrophy and electrical disturbances, including premature ventricular contractions, partial or complete atrioventricular block, and right bundle branch block. Death can result from arrhythmia or congestive heart failure. Sudden death occurs in 40% of congestive heart failure patients with Chagas’ disease. The second most commonly affected organ system is the gastrointestinal tract. The autonomic ganglia are destroyed, resulting in functional denervation, impaired motility, and thus dilation, leading to megaesophagus and megacolon.
Congenital Chagas’ disease is characterized by hepatosplenomegaly, sepsis, myocarditis, and hepatitis; however, two-thirds of cases of congenital Chagas’ disease are asymptomatic. Thus, routine testing for disease in the infants of infected mothers is warranted.
Acute infection and reactivation of infection in immunosuppressed transplant recipients and in HIV-infected patients can result in more severe clinical signs, sometimes involving the CNS. In HIV patients, reactivation has led to cerebral abscesses.
Diagnosis
The diagnosis of acute Chagas’ disease is made by detecting parasites in the blood, by using a wet preparation of anticoagulated blood or buffy coat or by using a Giemsa-stained smear of the blood.
Both enzyme immunoassay and ELISA tests are available commercially and are approved by the US Food and Drug Administration for the diagnosis of Chagas’ disease. False-positive results using these tests are an ongoing challenge, because there is cross-reactivity among patients with syphilis, malaria, leishmaniasis, and other parasitic diseases. PCR tests are also actively being studied and evaluated, although they are not yet available for routine clinical use. Serum samples can be sent to the CDC for indirect immunofluorescence and complement fixation testing (phone: [770] 488-4414).
Treatment
Acute American trypanosomiasis should be treated with nifurtimox (Box 3). In the United States, this drug is available through the CDC (phone: [404] 639-3670). A parasitologic cure using nifurtimox has been noted in 70-95% of parasitemic patients, but clinical cures are less well defined. Side effects with this drug occur in ~ 40-70% of adult patients and primarily include CNS problems such as disorientation, insomnia, paresthesias, seizures, and polyneuritis, as well as gastrointestinal symptoms including nausea, vomiting, and abdominal pain. Additionally, skin rash has been commonly noted.
Treatment of chronic infections and patients with end-organ damage includes supportive care. For example, pacemakers for cardiac conduction defects are sometimes indicated in this setting. Antiparasitic treatment is not indicated in chronic disease.
Prevention & Control
Disease control is directly related to the control of vectors (Box 4). Because of the potential chronic and insidious nature of this disease, some authorities recommend serologic screening of all persons at high risk who come from endemic areas. Such screening may have two benefits: (1) cardiac disturbances can often be treated with pacemakers, and (2) congenital disease can be prevented or treated.
The safety of the blood supply is a concern in endemic areas and in other regions with immigrants from endemic areas, such as southern California. Two approaches include screening and rejection of donors based on risk factors such as prolonged residence in an endemic area and based on serology. Some endemic countries such as Brazil now use routine serologic screening and reject blood based on positive results.
Travelers to endemic areas are advised to avoid sleeping in structures that may harbor the insect vector and to use appropriate barriers to avoid contact with the insects.