Description of Medical Condition
Pulmonary fungal infection endemic to the Southwest USA. Can become progressive and involve extrapulmonary sites, including bone, CNS, and skin. Known as the “great imitator.” Incubation period is 1 to 4 weeks after exposure.
System(s) affected: Pulmonary, Nervous, Musculoskeletal, Skin/Exocrine, Endocrine/Metabolic Genetics: Unknown Incidence/Prevalence in USA: 100,000 cases per year. (0.5% extrapulmonary)
Predominant age: All ages
Predominant sex: Male = Female
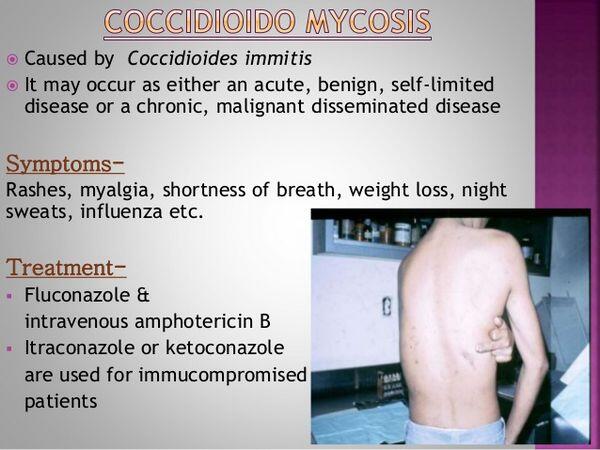
Medical Symptoms and Signs of Disease
Note: Over half of cases are subclinical
- Anorexia
- Arthralgias
- Chest pain
- Chills
- Confusion
- Cough, dry or productive
- Cyanosis
- Dyspnea
- Erythema nodosum
- Fatigue
- Fever
- Headache
- Malaise
- Night sweats
- Rash
- Sore throat
- Tenosynovitis
- Toxic erythema
- Weight loss
- Hepatomegaly; rare
- Hydrocephalus
- Hyperreflexia
- Pleural friction rub
- Splenomegaly; rare
- Tachycardia
What Causes Disease?
Coccidioides immitis, a soil fungus especially adapted to arid conditions. Liberated spores are inhaled when soil is disturbed: digging, construction sites, archaeological sites, dust storms, spelunking (exploring caves).
Risk Factors
- Certain groups are more prone to dissemination: immunocompromised hosts, pregnant women, African-Americans, Filipinos
- CNS involvement more common in young white males
- Immunosuppression. Previously infected patients can experience relapse years later through the mechanism of cell-mediated immune deficiency.
- Diabetes mellitus
- AIDS
- Chronic steroid use
Diagnosis of Disease
Differential Diagnosis
- Pneumonia, all etiologies
- Lung carcinoma
- Sarcoidosis
- Histoplasmosis, other fungi
- Lung abscess
- TB
- Lymphoma
- Meningitis
- Plus all other causes of cough, fever, fatigue
- Old granulomas can be mistaken for tumors
Laboratory
- Skin test turns positive at 3 weeks to 3 months; may remain positive indefinitely; applying skin test will not interfere with serologies. Skin test is currently not being manufactured and it is unclear when it will be available again.
- Serology — immunodiffusion measures precipitin antibodies (IgM) rise within 2 weeks and fall after 2 months; complement fixation antibodies (IgG) rise at 1-3 months; patients with mild symptoms may never develop detectable serology
- May have elevated sedimentation rate and peripheral eosinophilia
- Culture of sputum, wound exudate, joint aspirate; unlikely to grow fungus in urine, blood, pleural fluid
Drugs that may alter lab results: Steroids may alter ability to react to skin testing Disorders that may alter lab results: N/A
Pathological Findings
Fungal elements, spherules, seen best with H&E staining
Special Tests
Biopsy of affected tissue, e.g., lung nodule, skin lesion
Imaging
Chest x-ray findings include — normal, infiltrate(s), nodule(s), cavity, adenopathy mediastinal or hilar, pleural effusion
Diagnostic Procedures
If unable to establish diagnosis from skin testing and serologies — bronchoscopy, fine-needle biopsy, open lung biopsy, pleural biopsy, bone/skin/node biopsy, CSF stain, serology, culture
Treatment (Medical Therapy)
Appropriate Health Care
- Outpatient except in very severe cases
- Recommend referral to pulmonary or infectious disease specialist if drug treatment becomes imperative. Consider such treatment if IgG titers > 1:16, if disease persists without improvement over 6 weeks, or if skin test remains negative in the face of positive serology.
General Measures
- Cool mist humidifier for dry cough or sore throat
- Rest
- Supportive therapy
Activity
As tolerated
Diet
No special diet
Patient Education
For patient education materials favorably reviewed on this topic, contact: American Lung Association, 1740 Broadway, New York, NY 10019, (212)315-8700
Medications (Drugs, Medicines)
Drug(s) of Choice
- In mild cases, treat for symptomatic relief of cough with antitussives plus treat pleuritic pain with non-steroidal anti-inflammatory agents
- For persistent, progressive, or disseminated disease the following drugs are indicated. However, dosing, whom to treat, and length of treatment is controversial.
- Amphotericin B: 0.5-1.0 mg/kg with a total cumulative dose of 2-4 gm
- Ketoconazole: 400 mg/day
- Fluconazole: 400 mg/day. Fluconazole is also the treatment of choice for coccidioidomeningitis with a usual dose of 800 mg/day.
- Itraconazole: 200 mg bid
Contraindications: Avoid steroids Precautions: Amphotericin is highly nephrotoxic. Significant possible interactions:
- Ketoconazole-H2 blockers: decrease absorption of ketoconazole (ketoconazole requires an acidic pH for absorption).
- Azole antifungals — QT prolongation and ventricular arrhythmias
Alternative Drugs
N/A
Patient Monitoring
- If serology negative but index of suspicion is high, repeat every 2 weeks (skin test currently not available). With positive serologies, follow titers every 2 weeks until titers are dropping and patient has clinical improvement or resolution.
- Follow abnormal chest x-rays until findings are resolved or scarring process is complete
Prevention / Avoidance
- Not contagious between host and contacts
- Cultures in lab are highly contagious via inhalation and lab personnel must be very cautious when handling specimens
- High risk populations (see Risk Factors) should consider avoiding high risk activities, such as construction, archaeological digs, etc.
Possible Complications
- Severe cases are fatal, especially if associated with meningitis. Can cause destruction of pulmonary tissue due to scarring, cavities, etc.
- Hemoptysis
Expected Course / Prognosis
- Most cases are self-limited, resolve within a few months. Progressive and disseminated disease can be difficult to eradicate.
- Prognosis poor if weak cell mediated immunity response or high IgG
- Relapse of extrapulmonary or disseminated disease is common.
Miscellaneous
Associated Conditions
N/A
Age-Related Factors
Pediatric: N/A Geriatric: N/A
Pregnancy
Increased risk for dissemination, especially if contracted late in gestation
Synonyms
- Cocci
- Desert fever
- Posada-Wernicke disease
- Valley fever
- San Joaquin fever
International Classification of Diseases
114.9 Coccidioidomycosis, unspecified
See Also
Other Notes
Travel history is essential when working up any pulmonary infection not responding to normal measures. Rarely reported to be found in prostate, kidney, and endocrine glands.



