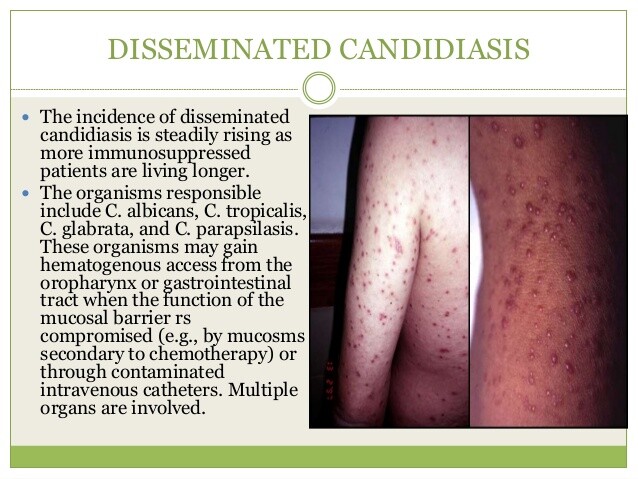
Candidemia may present in a variety of fashions, ranging from asymptomatic to fulminant sepsis. The candidemic patient generally has risk factors for infection, such as malignancy, chemotherapy-induced neutropenia, organ transplantation, GI surgery, burns, indwelling catheters, or exposure to broad-spectrum antibiotics.
Disseminated candidiasis must be assumed to be present in those with positive blood cultures, although negative cultures do not preclude the possibility of disseminated disease. Dissemination usually manifests with many microabscesses involving multiple organs, especially the liver, spleen, and eye, but almost any organ may be involved (Box 2).
Diagnosis
Candidemia is diagnosed by recovering Candida species in blood culture. Candidemia may be isolated or may occur in the setting of disseminated candidiasis. The possibility of disseminated candidiasis should be considered in any patient with deep Candida infection, multiple sites of infection, or positive blood cultures. Disseminated candidiasis is diagnosed by tissue culture of biopsy material or demonstration of Candida in histologic specimens. At present, serology is available but has false-negative and false-positive rates too high to be of use clinically.
Treatment
The treatment of candidemia is the subject of much debate and controversy. Because isolation of Candida from the blood carries a high morbidity and because there is currently no method to predict which patients will not require treatment, there is agreement that all patients with candidemia should be treated. The standard treatment in the past has been amphotericin B, with or without 5-FC. Currently, fluconazole appears to be a reasonable alternative, although there are limited data comparing mortality of fluconazole-treated patients versus those treated with amphotericin. One randomized study of candidemic patients demonstrated fluconazole to be equally efficacious but associated with less toxicity when compared with amphotericin.
Fluconazole may be used as initial treatment of candidemia in a stable patient (Box 73-7). If patients had been treated with fluconazole for 2 days or greater at the time of candidemia, deteriorate on fluconazole therapy, or are unstable (hypotension, need for mechanical ventilation, multiple comorbid factors, etc.) at the time their candidemia is diagnosed, then treatment with amphotericin is warranted. Smaller doses may be used if amphotericin if chosen as the initial regimen for stable patients. Because of the potential bone marrow toxicity of 5-FC, particularly when combined with amphotericin, the dose of 5-FC is generally reduced when part of the treatment regimen. Treatment is generally continued until clinical improvement is seen and for 2 weeks after the last positive blood culture.
For all patients with candidemia, the possibility of disseminated infection must be considered. If infection with C krusei is suspected or documented, fluconazole should not be used as initial therapy because this species has a high level of resistance to fluconazole. C glabrata has an intermediate level of resistance, and fluconazole therapy may be used with caution. Clinical deterioration should prompt an early change of therapy to amphotericin. Treatment for disseminated disease should continue until there is definite resolution of parenchymal involvement and for 2 weeks after the last positive blood culture.
Intravenous catheters should be removed from candidemic patients if possible. In addition, all patients with candidemia should be followed clinically for at least 3 months, as deep infection caused by hematogenous spread may not manifest initially. Patients should be instructed to report any symptoms, which may represent late complications, such as fever, fatigue, jaundice, visual disturbances, abdominal pain, or bone pain.
Links
https://www.uptodate.com/contents/chronic-disseminated-candidiasis-hepatosplenic-candidiasis
http://www.pharmacytimes.com/publications/issue/2006/2006-03/2006-03-5329