The clinical signs and symptoms of meningitis are variable (See Table Mean Values of the Components of Normal and Abnormal Cerebrospinal Fluid).
General
- Clinical presentation varies with age, and generally, the younger the patient, the more atypical and the less pronounced is the clinical picture.
| TABLE. Mean Values of the Components of Normal and Abnormal Cerebrospinal Fluid | ||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||
- Up to 50% of patients may receive antibiotics before a diagnosis of meningitis is made, delaying presentation to the hospital. Prior antibiotic therapy may cause the Gram stain and cerebrospinal fluid culture to be negative, but the antibiotic therapy rarely affects cerebrospinal fluid protein or glucose.
Signs and symptoms
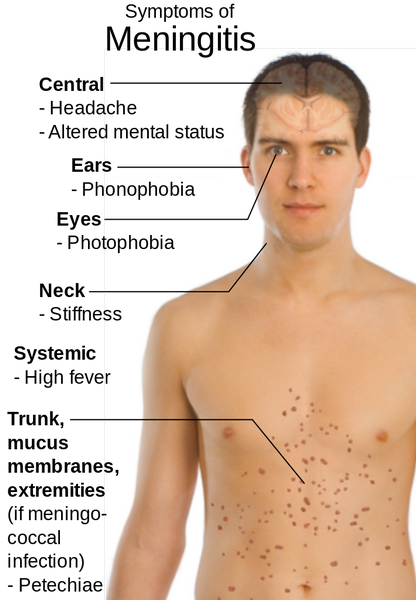
- Classic signs and symptoms include fever, chills, vomiting, photophobia, severe headache, and nuchal rigidity associated with Kernig’s and Brudzinski’s signs. Kernig’s and Brudzinski’s signs are poorly sensitive and frequently are absent in children.
- Other signs and symptoms include irritability, delirium, drowsiness, lethargy, and coma.
- Clinical signs and symptoms in young children may include bulging fontanelle, apneas, purpuric rash, and convulsions in addition to those just mentioned.
- Seizures occur more commonly in children (20% to 30%) than in adults (0% to 12%).
Differential signs and symptoms
- Purpuric and petechial skin lesions typically indicate meningococcal involvement, although the lesions may be present with H. influenzae meningitis. Rashes rarely occur with pneumococcal meningitis.
- Waterhouse-Friderichsen syndrome, a rapid eruption of multiple hemorrhagic lesions associated with a shocklike state, is associated with meningococcal meningitis.
- H. influenza meningitis and meningococcal meningitis both can cause involvement of the joints during the illness.
- A history of head trauma with or without skull fracture or presence of a chronically draining ear is associated with pneumococcal involvement.
Laboratory tests
- Several tubes of cerebrospinal fluid are collected via lumbar puncture for chemistry, microbiology, and hematology tests. Theoretically, the first tube has a higher likelihood of being contaminated with both blood and bacteria during the puncture, although the total volume is more important in practice than the tube cultured. cerebrospinal fluid should not be refrigerated or stored on ice.
- Analysis of cerebrospinal fluid chemistries typically includes measurement of glucose and total protein concentrations. An elevated cerebrospinal fluid protein of 100 mg/dL or greater and a cerebrospinal fluid glucose concentration of less than 50% of the simultaneously obtained peripheral value suggest bacterial meningitis.
- The values for cerebrospinal fluid glucose, protein, and white blood cell concentrations found with bacterial meningitis overlap significantly with those for viral, tuberculous, and fungal meningitis Therefore, cerebrospinal fluid white blood cell counts and cerebrospinal fluid glucose and protein concentrations cannot always distinguish the different etiologies of meningitis.
Other diagnostic tests
- Blood and other specimens should be cultured according to clinical judgment because meningitis frequently can arise via hematogenous dissemination or can be associated with infections at other sites. A minimum of 20 mL of blood in each of two to three separate cultures per each 24-hour period is necessary for the detection of most bacteremias.
- Gram stain and culture of the cerebrospinal fluid are the most important laboratory tests performed for bacterial meningitis. The Gram stain continues to be the most rapid and accurate method of presumptively diagnosing acute bacterial meningitis. When performed before antibiotic therapy is initiated, Gram stain is both rapid and sensitive and can confirm the diagnosis of bacterial meningitis in 75% to 90% of cases. The sensitivity of the Gram stain decreases to 40% to 60% in patients receiving prior antibiotic therapy. Culture is required to differentiate the various bacterial etiologies.
- Polymerase chain reaction techniques can be used to diagnose meningitis caused by N. meningitidis, S. pneumoniae, and Hib. Polymerase chain reaction is considered to be highly sensitive, but use of this diagnostic approach is limited owing to expense.
- Latex fixation, latex coagglutination, and enzyme immunoassay tests provide for the rapid identification of several bacterial causes of meningitis, including S. pneumoniae, N. meningitidis, and Hib. Rapid-identification latex tests work by bringing potential capsular antigens of the pathogen causing meningitis in contact with a specific antibody, causing an antigen-antibody reaction. This capsular antigen-antibody reaction can be observed visually and quickly without waiting for culture results. The rapid antigen tests should be used in situations in which the Gram stain is negative. The sensitivity and specificity of latex fixation and coagglutination tests can vary with the manufacturer of the antibody, density of the antigen present in the cerebrospinal fluid, and pathogen being tested.
- Diagnosis of tuberculosis meningitis employs acid-fast staining, culture, and Polymerase chain reaction of the cerebrospinal fluid.
- Polymerase chain reaction testing of the cerebrospinal fluid is the preferred method of diagnosing most viral meningitis infections.
- The standard diagnostic tests for fungal meningitis include culture, direct microscopic examination of stained and unstained specimens of cerebrospinal fluid, antigen detection of cryptococcal or histoplasmal antigens, and antibody assay of serum and/or cerebrospinal fluid.
Desired outcome
The goals of treatment include eradication of infection with amelioration of signs and symptoms, and prevention of neurologic sequelae, such as seizures, deafness, coma, and death.


