Description of Medical Condition
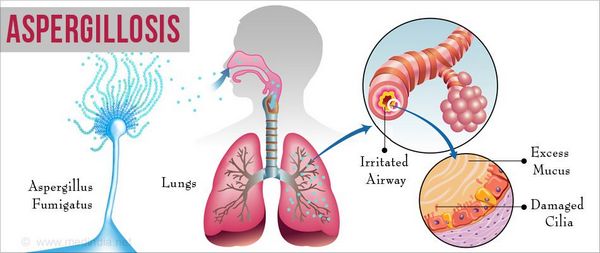
Disease caused by a ubiquitous mold that primarily involves the lungs. Disease frequently lethal in neutropenic and bone marrow transplant (BMT) patients. Syndromes include:
- Allergic aspergillosis
- Extrinsic allergic alveolitis — hypersensitivity pneumonitis in individuals repeatedly exposed to the fungus
- Allergic bronchopulmonary aspergillosis (ABPA)
- pulmonary infiltrates, mucous plugging; secondary to allergic reaction to fungus
- Aspergillomas: “fungus ball” saprophytic colonization within pre-existing pulmonary cavities
- Invasive aspergillosis: most common and severe in BMT and neutropenic patients. Also occurs with increased frequency in other immunocompromised persons, such as those with AIDS, solid organ transplant or high dose corticosteroids; commonly fatal.
System(s) affected: Pulmonary, Nervous, Gastrointestinal, Musculoskeletal, Cardiovascular
Genetics: No known genetic pattern
Incidence/Prevalence in USA: Rare
Predominant age: None
Predominant sex: Male = Female
Medical Symptoms and Signs of Disease
- Allergic — cough, wheezing, constitutional symptoms, plug expectoration
- Aspergillomas — hemoptysis; manifestations of underlying disease
- Invasive — fever, cough, rales, rhonchi; toxicity; CNS signs; Gl bleeding
What Causes Disease?
Aspergillus species in decreasing order of frequency: A. fumigatus, A. flavus, A. niger
Risk Factors
- Allergic — exposure, asthma
- Aspergillomas — COPD, bronchiectasis, TB, malignancy
- Invasive — neutropenia, corticosteroid therapy, graft vs. host disease in recipients of bone marrow transplant. AIDS
Diagnosis of Disease
Differential Diagnosis
- Allergic — other causes of asthma and hypersensitivity pneumonitis.
- Aspergillomas — neoplasm, TB
- Invasive — bacterial pneumonia, pulmonary hemorrhage, drug toxicity, malignancy; mucor (sinuses).
Laboratory
- ABPA — eosinophilia, immediate skin reactivity to aspergillus antigen, precipitating-serum antibodies to aspergillus, elevated serum IgE concentrations.
- Invasive — sputum culture, cultures of bronchoalveolar lavage or bronchial washings; biopsy is definitive; blood cultures almost never positive
Drugs that may alter lab results: None
Disorders that may alter lab results: None
Pathological Findings
Necrotiz ing pneumonia, hemorrhagic infarcts, bloodvessel invasion; branching septate hyphae if organism seen microscopically
Special Tests
- ABPA — immediate skin reactivity to aspergillus antigen, precipitating serum antibodies (precipitins) against aspergillus antigens, elevated serum IgE concentrations, elevated serum IgE and IgG antibodies specific to A. fumigatus.
- Invasive — none
Imaging
Chest x-ray — fleeting infiltrates (ABPA), round intracavity mass (aspergillomas); nodular or patchy infiltrates progressing to diffuse consolidation and cavitation (invasive); nodular, cavitary or pleural-based wedge-shaped lesions
Diagnostic Procedures
Bronchos copy, bronchial washings, bronchoalveolar lavage or transthoracic needle aspiration may be helpful in isolating organism in invasive disease; open lung biopsy is diagnostic but often not possible in severely ill, ventilated patients.
Treatment (Medical Therapy)
Appropriate Health Care
- Allergic — outpatient usually
- Aspergillomas — outpatient usually
- Invasive- inpatient
General Measures
- Allergic
- Extrinsic allergic alveolitis -drug therapy, exposure avoidance. OABPA-corticosteroids
- Aspergillomas – individualized therapy ranging from no therapy to surgical resection of cavities in cases of severe hemoptysis; systemic antifungal therapy is seldom useful
- Invasive – (prognosis tends to be poor) high dose intravenous antifungal therapy; treatment of underlying disease; adjunctive cytokine therapy to reverse neutropenia
Activity
As tolerated
Diet
No special diet
Patient Education
To specifics of individual circumstances.
Medications (Drugs, Medicines)
Drug(s) of Choice
- Allergic
- Extrinsic allergic alveolitis — bronchodilators, cromolyn, steroids
- ABPA-steroids
- Aspergillomas — none
- Invasive — high dose amphotericin B — up to 1 mg/kg/ day. The lipid formulations of amphotericin B (Abelcet. Ambisome) are preferred over standard amphotericin because of the reduced nephrotoxicity in view of the high doses required.
- Caspofungin is approved for patients with aspergillosis unresponsive to other therapy or who have unacceptable toxicity to other agents
- Voriconazole was superior to conventional amphotericin in a large study and is well absorbed orally
- Note: because of the frequent failure of single drug therapy, combination therapy is frequently proposed
Contraindications: Refer to manufacturer’s literature
Precautions: Amphotericin B can cause significant renal insufficiency and electrolyte abnormalities. Saline infusion at the time of amphotericin B administration may decrease the nephrotoxicity.
Significant possible interactions:
- Amphotericin B — other nephrotoxic drugs (aminoglycosides, cyclosporine, etc): accelerate development of renal insufficiency
- Amphotericin B — diuretics: accelerate electrolyte depletion
- Voriconazole — hepatically metabolized drug; serum levels may be altered
- Itraconazole-hepatically metabolized drugs: serum levels altered
- Itraconazole — gastric pH: normal, low pH is necessary for absorption
Alternative Drugs
Itraconazole is occasionally useful as an alternative agent
Patient Monitoring
- Allergic
- Extrinsic allergic, alveolitis — spirometry
- ABPA — chest x-ray, IgE levels
- Aspergillomas — chest x-ray, symptoms
- Invasive — chest x-ray, CBC
Prevention / Avoidance
- Allergic — avoid exposure
- Aspergillomas — treatment of underlying diseases, eg. COPD, etc.
Possible Complications
- Allergic- bronchiectasis, pulmonaryfibrosis, obstructive lung disease
- Aspergillomas — hemoptyses
- Invasive — metastatic infection of CNS, Gl tract and other organs; death
Expected Course / Prognosis
- Allergic — with treatment prognosis is good; untreated can progress to severe fibrosis, COPD
- Aspergillomas — prognosis more related to underlying disease
- Invasive — poor prognosis
Miscellaneous
Associated Conditions
- Allergic — asthma
- Aspergillomas — COPD, TB, pulmonary mycoses, silicosis, sarcoidosis, non-tuberculosis mycobacteria, ankylosing spondylitis, malignancy
- Invasive- neutropenia

Age-Related Factors
Pediatric: N/A
Geriatric: N/A
Others:
- Allergic — Tends to occur in younger patients <35.
- Aspergillomas — older patients with chronic lung disease
- Invasive-all ages
Pregnancy
N/A
Synonyms
- Hypersensitivity pneumonitis
- Fungus ball
International Classification of Diseases
117.3 Aspergillosis
Abbreviations
ABPA:
monary aspergillosis
allergic bronchopul




