Essentials of Diagnosis
- Suspected in patients with fever, lymphadenopathy, and skin lesions who have a history of animal exposure (including to wild animals, ticks, or deerflies) or are coming from a high prevalence area or in laboratory personnel who work with Francisella spp.
- Blood culture or other biologic specimen cultures on appropriate culture media.
- Serum antibody titer = 1:160 or a fourfold increase or decrease in titer.
General Considerations
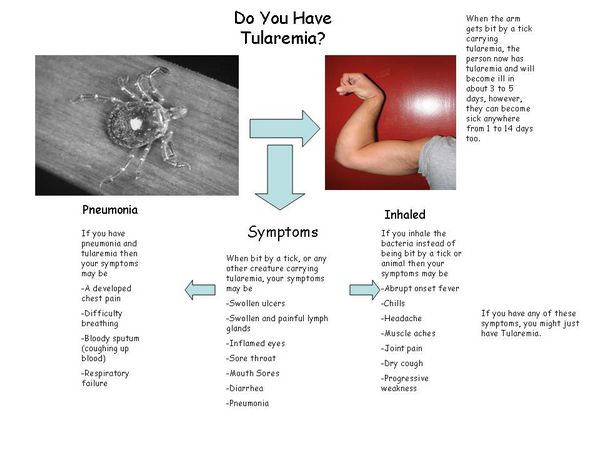
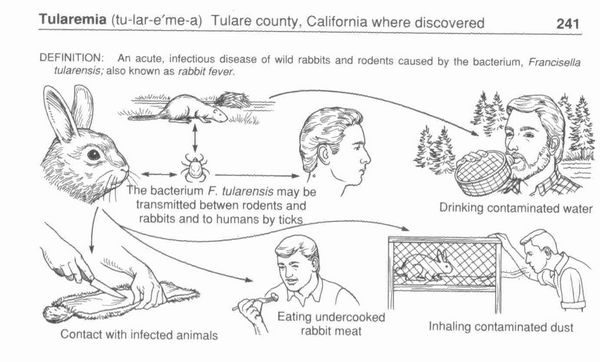
Francisella tularensis is the causative agent of tularemia (also called rabbit fever or deerfly fever), an infectious disease that occurs primarily in animals. It may occasionally cause human disease, which most often manifests itself by one or more skin lesions, regional lymphadenopathy, fever, and constitutional symptoms.
Epidemiology
Tularemia is widely distributed, with a higher prevalence in the northern hemisphere. Once common before World War II in the United States, the incidence of tularemia has declined steadily since the 1950s. Currently, the incidence is 0.05-0.15 cases/100,000 population. More than one-half of the cases in the United States occur in Missouri, Arkansas, Oklahoma, Texas, and Illinois. The incidence is higher during the summer months because of the increase in tick-acquired disease.
Transmission of F tularensis to humans occurs through dermal or mucosal contact with infected animals, mainly wild mammals, amphibians, fish, birds, or as the result of an insect bite (eg, ticks, deerflies, and mosquitoes). In the United States, the most common reservoirs are rabbits and ticks. Occasionally, the infection is acquired through inhalation of aerosolized organisms. The organism is highly infectious for laboratory personnel.
Microbiology
F tularensis is a small aerobic, nonmotile, catalase-positive pleomorphic gram-negative coccobacilli. The cell wall of F tularensis is high in fatty acids. Some strains contain a lipid-rich capsule that increases virulence. F tularensis requires a sulphudryl-containing medium for growth and, therefore, does not grow on most routine commercially available media. Growth requires 2-4 days and produces small, smooth, opaque colonies. The organism may be identified on the basis of its morphology, growth requirements, fluorescent staining, and agglutinins with specific antisera. Most strains are ß-lactamase producers.
Pathogenesis
After contact with the microorganisms, penetration occurs through sites of inapparent skin disruption. Subsequently, F tularensis multiplies locally and in the skin produces papules that ulcerate, become encrusted, and form an eschar. The microorganisms then reach regional lymph nodes where they replicate and disseminate to the blood. The organisms are engulfed by cells of the reticuloendothelial system in which they may survive intracellularly for prolonged periods. Occasionally, the microorganisms are inhaled, and a pneumonic form of the disease occurs. Rarely, ingestion of the microorganisms can cause pharyngitis, cervical, and mesenteric lymphadenopathy. Early lesions are characterized histopathologically by focal necrosis occurring in organs of the reticuloendothelial system that subsequently undergo granulomatous reaction. Healing is associated with fibrosis and calcification of the granulomata.
Clinical Findings
Signs and Symptoms
The clinical manifestations of tularemia are protean and depend on the portal of entry of the microorganism, virulence of the microorganism, and the immune status of the human host. It can vary from a subclinical illness to a fulminant disease with sepsis and death. Five different clinical syndromes have been described (Box 4). The incubation period is 3-5 days.
In the most common form of infection, the ulceroglandular type, a red, tender cutaneous papule is noted at the site of an insect bite or dermal penetration with ulceration on the affected limb and concomitant tender regional adenopathy. The ulcer becomes crusted and black-colored, forming an eschar, which is a characteristic feature of the cutaneous site of entry. Symptoms include fever (39-40.6 °C), chills, headaches, and generalized malaise. Patients often are acutely ill with severe prostration and occasionally hypotension, septicemia, and death. If untreated, fever may persist for a month or longer. On physical examination, the temperature elevation is often associated with a paradoxically relative bradycardia. Hepatosplenomegaly is common, especially in untreated cases.
Tularemia should be suspected in febrile patients with skin lesions and lymphadenopathy especially when a history of contact with wild animals, ticks, or deerflies is present.
Laboratory Findings
Organisms are rarely seen on Gram stain of affected tissue. Blood cultures or other biologic specimens need special culture media for growth. Serologic studies using the microagglutination test, or the enzyme immunoassay test, are reliable and widely available. A fourfold increase or decrease in the titers is diagnostic of infection. A titer of = 1:160 may represent recent or acute infection. As many as 50% of cases will have positive titers by the second week of the illness. Titers may remain elevated for months to years after an acute infection.
Imaging
In 30% of cases, a chest roentgenogram will show infiltrates, despite normal clinical findings. Typical chest roentgenogram findings in the pneumonic form would include lobar or subsegmental infiltrates, hilar adenopathy, or diffuse infiltrates.
Differential Diagnosis
The differential diagnosis of the ulceroglandular form is one of other diseases that are associated with skin ulcer and lymphadenopathy, such as pyoderma caused by streptococci or staphylococcus, sporotrichosis (Sporothrix schenckii), cat-scratch disease, rat-bite fever, plague, anthrax, brucellosis, typhoid fever, infectious mononucleosis, and hematologic malignancies.
Complications
The most common complication is suppuration of an involved lymph node. Other complications such as meningitis, osteomyelitis, endocarditis, and peritonitis occur rarely.
Treatment
Aminoglycosides, mainly streptomycin or gentamicin, are considered the drugs of choice for all forms of tularemia (Box 5). Other antimicrobial agents such as tetracyclines and chloramphenicol have been used in patients who cannot tolerate aminoglycosides. Their bacteriostatic effect against F tularensis may account for the high relapse rates. Relapse is not caused by resistant microorganisms and may be treated with another course of the same antimicrobial regimen.
Prognosis
Immunity after infection with F tularensis is lifelong. The mortality rate is 5-15% in untreated cases and 1% in treated cases. The typhoidal form is associated with a high mortality rate.
Prevention & Control
Avoidance of exposure to contact with potential sources of infection is the best means of prevention (Box 6). Gloves, masks, and goggles should be worn when handling potentially infected animals. A live attenuated vaccine is available for individuals at high risk such as veterinarians and meatpacking plant employees.




