The toxic shock syndrome (TSS) is a heterogeneous complex of symptoms attributed to TSST-1 toxin-producing S aureus. Two variants have been described: menstruation-associated and nonmenstrual disease. Cases of menstruation-associated disease are correlated with the use of superabsorbent tampons. Diaphragm contraception, parturition, indwelling foreign bodies, and recent surgery predispose to nonmenstrual disease.
Clinical Findings
Signs and Symptoms
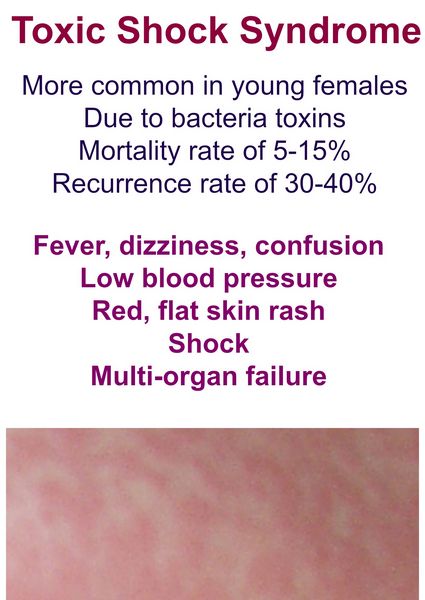
Myalgias, headache, malaise, watery diarrhea, and confusion (in the face of a normal neurologic exam) are early symptoms of TSS, typically preceding the rash by 2-3 days. Erythroderma is initially seen on the palms and soles, progressing to a confluent generalized rash. Hypotension and fever are invariably present at this stage. Multisystem organ failure may be present early or late in the disease course. Dermal desquamation, particularly of the palms and soles is a late sequela of TSS, occurring 7-14 days after the onset of symptoms.
Laboratory Findings
The laboratory abnormalities in TSS reflect the diverse organ systems involved. Laboratory abnormalities included as criteria for case definition (see Table 3) include an elevation in creatine phosphokinase, acute renal insufficiency, sterile pyuria, elevated liver function tests, and thrombocytopenia. Disordered electrolytes (particularly hypocalcemia and hypophosphatemia), neutrophil predominance on white blood cell differential, and anemia, while not explicitly mentioned in the case definition, may also be found in patients with TSS.
Differential Diagnosis
Other entities causing rash, hypotension, or fever that may be confused with staphylococcal TSS include streptococcal TSS, Rocky Mountain spotted fever, viral infection with exanthem (such as measles or EBV), meningococcemia, leptospirosis, the septic shock syndrome, Kawasaki’s disease, and drug-induced reactions (such as erythema multiforme or toxic epidermal necrolysis). A thorough history with particular attention to tick exposures, ill contacts, travel, pets, and medication use is essential in excluding the mimicking conditions.
Complications
Case fatality rates for TSS range from 3% to 6% and are higher for nonmenstrual disease. Digital gangrene may occur as a result of sustained hypotension and impaired extremity perfusion. Neuropsychiatric symptoms such as emotional lability, impaired memory, and decreased concentration are common sequelae in survivors.
Diagnosis
Formal criteria for the diagnosis of TSS have been developed to facilitate surveillance and standardize case definition (Table 3). Increased awareness of the association between menstruation, tampon use, and TSS has led to improved diagnosis of menstruation-associated disease. Nonmenstrual disease lacks unifying epidemiologic characteristics, which makes diagnosis more difficult. Postoperative TSS is particularly difficult to diagnose, as surgical wound inflammation may be minimal, and early signs are nonspecific.
The diagnosis of TSS is supported by a culture of TSST-1-producing S aureus from an infected focus, although this is not a criterion for case definition. TSST-1-producing staphylococci are isolated from the vagina in 85% of menstruation-associated disease but are isolated from infected foci in only 40-60% of cases of nonmenstrual disease. S aureus bacteremia rarely occurs with TSS.
Treatment
Treatment requires identification and removal of foreign bodies (such as tampons) and irrigation and debridement of infected wounds. Aggressive hydration and close hemodynamic monitoring are essential in the early stages of TSS. All patients should be treated with parenteral agents active against staphylococci (Box 3). In vitro, clindamycin inhibits TSST-1 protein synthesis, providing at least a theoretical basis for combination therapy with this agent and a penicillinase-resistant penicillin.


