Essentials of Diagnosis
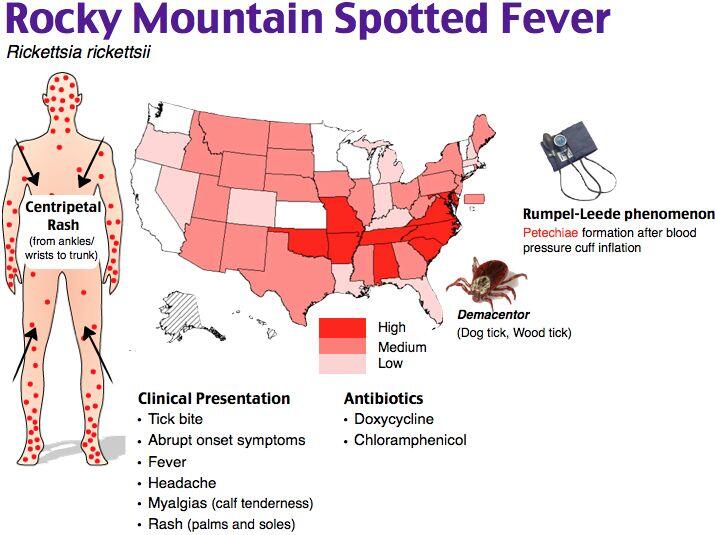
- Key symptoms and signs: abrupt onset of high fevers, headaches, myalgias, malaise, and a flu-like illness 3-12 days after tick bite; rash (80-90% of patients, initially maculopapular, then petechial, classically involving the palms and soles).
- Predisposing factors: tick exposure (April through September), pet owners, animal handlers, and outdoor activities.
- Commonest geographic location of infection: rural.
- Confirmatory serology via IFA.
- PCR with blood or skin biopsy: sensitive and specific but not widely available.
General Considerations
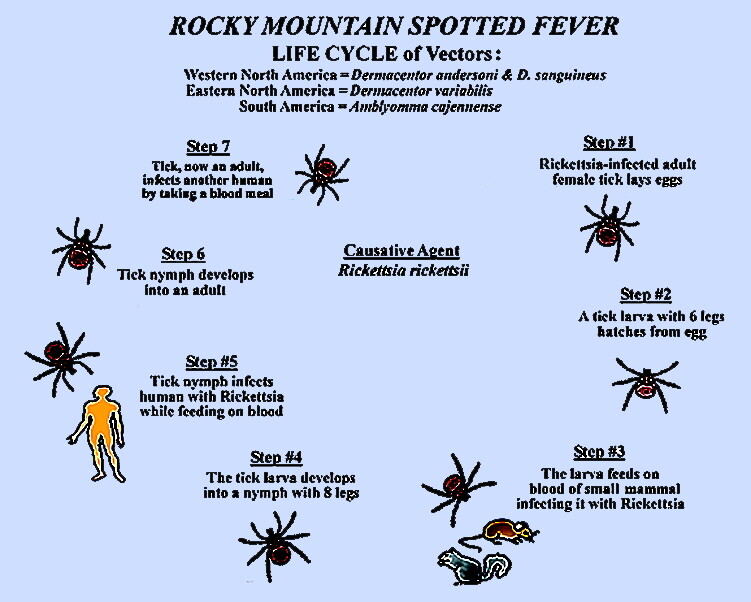
RMSF is caused by Rickettsia rickettsii and is an acute tick-borne illness occurring during seasonal tick activity. The disease is characterized by acute onset of fever, headache, and a rash of the extremities spreading to the trunk.
A. Epidemiology. Transmission of R rickettsii to humans by the Dermacentor tick occurs only if there is prolonged contact of at least several hours between the tick and the human host. RMSF is found only in the Western Hemisphere, with ~600 reported cases per year in the United States. Of those cases, ~50% occur in the mid-Atlantic states, but all states except Hawaii and Vermont have reported cases. Most (90%) of cases occur from April through September. Children in the 5- to 9-year age group have the highest incidence of infection. Another peak of disease incidence is observed among males >60 years of age.
Clinical Findings
A. Signs and Symptoms. Only 3% of cases present with the classic triad of fever, rash, and history of a tick bite. The incubation period is 3-12 days (average 7 days), which is then followed by abrupt onset of high fevers, headaches, malaise, and myalgias, followed by 1 to 2 days of a nonspecific flulike illness (Box 68-6). Early in the course of illness, chills, rigors, neck stiffness, anorexia, nausea, vomiting, and abdominal pain occur frequently. Conjunctival suffusion, photophobia, cough, and neurologic symptoms may also be present. In severe cases, mental confusion and obtundation may develop. Only 14% of patients with RMSF will have a rash on day 1, but, by day 3, 49% will have the characteristic rash. In 20% of cases, the rash occurs only after day 6, while 9-16% of patients will never develop a rash even though their illness is equally severe.
The initial rash of RMSF is erythematous and macular, involving the ankles and wrists. It then spreads to involve the palms, soles, trunk, and face. The rash becomes papular as local edema and perivascular inflammatory cell infiltrates accrue. The lesions are petechial in 41-59% of patients after day 6 of the illness if antibiotics are not administered early. The centripetal progression and the involvement of the palms and soles are the important diagnostic features. However, it is important to realize that, at day 3, at which time most people will present for care, the features considered most critical for rendering a diagnosis of RMSF are absent.
Gastrointestinal manifestations such as nausea, vomiting, diarrhea, and abdominal pain occur in 39-63% of patients. Liver involvement is frequently manifested by mild to moderate elevations of hepatic enzymes. Pulmonary findings in RMSF are the most worrisome. The pathology of lung biopsy specimens from infected patients is characterized by widespread endothelial damage. Neurological involvement is the most significant cause of morbidity and mortality in RMSF. Clinically evident encephalitis is seen in =28% of cases. Symptoms vary from confusion, lethargy, stupor, delirium, and ataxia to coma and convulsions. Of all patients, 30% will have lymphohistiocytic meningitis. The course of untreated RMSF is marked by slowly advancing severity of illness, with high temperatures plus hemorrhagic and neurologic signs.
B. Laboratory Findings. The leukocyte count is usually slightly decreased or normal, but an elevated band count of >10% is seen in 69% of patients. Thrombocytopenia occurs in 52% of patients, and 32% will have platelet counts of <100,000/ml3. Other abnormalities include hyponatremia and elevated serum aminotransferase and bilirubin levels.
C. Imaging. Pneumonitis and capillary endothelial injury can result in life-threatening noncardiac pulmonary edema which may be seen on chest x-ray.
D. Differential Diagnosis. The differential diagnosis of RMSF includes influenza, enteroviral infection, typhoid fever, leptospirosis, infectious mononucleosis, viral hepatitis, and bacterial sepsis — especially meningococcemia, HME, and HGE.
E. Complications. Fulminant RMSF (>5 days from onset to death) is seen more commonly in black male patients with glucose-6-phosphate dehydrogenase deficiency and in the elderly. For those patients with RMSF who are hospitalized for >2 weeks, ~50% will have long-term neurologic complications.
Diagnosis
Confirmatory serology is retrospective in nature; therefore, the physician must have a high index of suspicion based on clinical findings to start therapy. There are no diagnostic laboratory tests other than specific serologic and PCR-based tests. The leukocyte count is usually slightly decreased or normal, but an elevated band count of >10% is seen in 69% of patients. Thrombocytopenia occurs in 52% of patients, and 32% will have platelet counts of <100,000/ml3.
Other abnormalities include hyponatremia and elevated serum aminotransferase and bilirubin levels. A PCR assay for RMSF using whole blood is now available through state health departments or the Centers for Disease Control and Prevention. None of the currently available serologic tests are useful for diagnosis in the acute phase of illness. The most sensitive and specific serologic assay is an IFA test. A diagnostic titer of >64 is usually detectable between 7 and 10 days after the onset of symptoms.
The less sensitive latex agglutination test is more widely available and will demonstrate a rise in titer to >128, 7-9 days after the onset of symptoms. Immunohistologic examination by immunofluorescence or immunoenzyme staining for R rickettsii in skin biopsy specimens can demonstrate the presence of the organism as early as days 3-8 of the illness and has a reported sensitivity and specificity of 70% and 100%, respectively.
Treatment
Doxycycline is the drug of choice for the treatment of RMSF, except in cases of pregnancy and drug allergy or in children <9 years of age (Box 7). Although chloramphenicol has been recommended in these groups, many experts feel that it is safe to give a short course of doxycycline for the treatment of a potentially life-threatening infection in children <9 years old.
The likelihood of permanent tooth staining from a short course of doxycycline is very low. Although there are in vitro data indicating that fluoroquinolones may be efficacious, these agents have not been widely used in the treatment of RMSF and cannot be recommended at this time. Treatment is continued for =2 days after defervescence to reduce the risk of relapse. If therapy is started early, most patients defervesce within 48 to 72 h. Severely ill patients treated late in the course of disease may take considerably longer to recover.
Prevention
Avoidance of tick bites is the best method of prevention. Protective clothing, tick repellents, and careful total body inspection can reduce the risk of inoculation. Prompt removal of ticks with forceps by firm traction is the preferred method. It is essential not to crush the tick so as to prevent release of rickettsiae.
Read more
https://www.cdc.gov/rmsf/index.html
https://www.healthline.com/health/rocky-mountain-spotted-fever